48uep6bbphidvals|441
48uep6bbph|2000F98CTab_Articles|Fulltext
Biliary tract is an uncommon site for infestation by Ascaris
lumbricoides (round worm). In India biliary ascariasis is highly
prevalent in Kashmir valley because of climatic and soil
conditions.1-3 Only sporadic reports in the form of anecdotal
cases or small patient series have been reported from remaining
parts of the country.4-7 In this report we present our experience
of this entity, highlighting the possible predisposing factors,
clinical features and management.
Methods
All the patients with a diagnosis of biliary ascariasis were
analyzed from a prospectively managed database of all cases
admitted between April 2004 and April 2010. The diagnosis
was made on the basis of ultrasound and/or cholangiographic
findings and confirmed by detection of live worm in the bile
duct or descending duodenum (in the vicinity of ampulla of
Vater). The clinical features, laboratory parameters and
treatment of these patients were reviewed.
Results
A total of nine (two males and seven females) patients were
included in this study. The median age was 62 yrs (range 37 -
68 yrs). Six patients had prior cholecystectomy for symptomatic
cholelithiasis. Two of these patients had concomitant
choledocholithiasis that was treated with choledocholithotomy
and T tube drainage in one and lateral
choledochoduodenostomy (CDD) in another. The T tube
cholangiogram showed a retained stone in the common bile
duct (CBD) for which the patient was referred to our center for
endoscopic extraction. The remaining four patients at a later
date were detected to have retained CBD stones that were
treated by endoscopic sphincterotomy (ES) and stone
extraction. The median interval between diagnosis of biliary
ascariasis and sphincter ablative/ bypass procedure (ES or
CDD) was 14 months (range 6 months – 4 yrs). Three patients
presented without any prior history of biliary symptoms or
surgery. All but one patient presented with acute onset pain
abdomen predominantly located in the upper abdomen and
very typically radiating to back. The patients variously
described the pain as piercing, cutting or hammering in
character. Clinically the pain appeared to mimic a pancreatic
pathology except that it had a waxing and waning character
with minimal abdominal signs. The median duration of symptom
was 24 hrs (range 6 hr - 3 days). The patient with T Tube
choledochostomy who was otherwise asymptomatic had an
incidental detection of a worm on cholangiogram prior to
endoscopic extraction of the retained stone. All the patients
were anicteric and afebrile. Examination of the abdomen
revealed mild epigastric tenderness in five patients. One patient
with intact gallbladder had positive ‘Murphy’s sign’ suggesting
acute cholecystitis. In the remaining patients clinical diagnosis
of biliary colic or acute pancreatitis was entertained. Laboratory
investigations showed normal differential and total eukocyte
counts in all cases. The liver function tests (serum bilirubin,
aminotransferase, alanine transferase and alkaline phosphatase)
were normal except in two patients in whom the liver enzymes
showed mild elevation. Serum amylase was normal in all the
symptomatic patients. Ultrasound examination of abdomen
revealed a dilated CBD in eight patients. A linear echogenic
structure suggestive of round worm was reported in the CBD
in six of these patients. Features suggestive of acute
cholecystitis were present in one patient. All the patients were
subjected to endoscopic retrograde cholangiogram (ERC) with
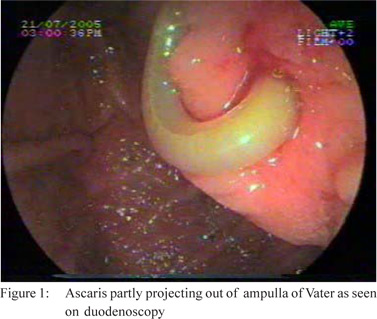
a diagnostic and therapeutic intent. In one patient part of the
round worm was seen partially projecting out of the papilla of
Vater (Figure 1). After extraction of this worm, CBD
opacification was performed that showed dilatation but no filling
defect. In two patients only dilated CBD was noted but live
worm(s) were found in the descending part of duodenum
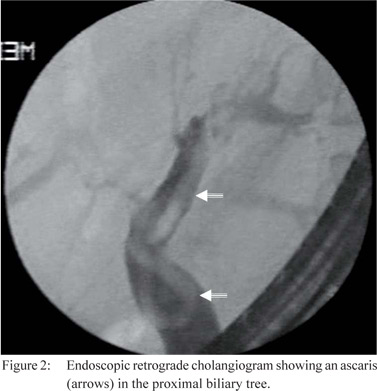
suggesting their possible migration out of the bile duct. In five
patients curvilinear filling defects suggestive of round worm(s)
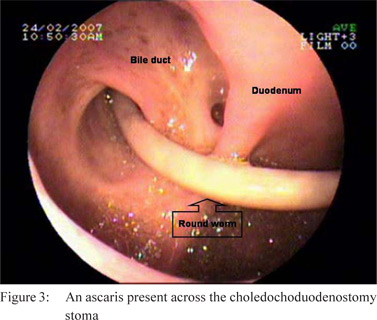
were noted in the CBD (Figure 2). In the lone patient with
choledochoduodenostomy, a live worm was found across the
stoma partly inside the CBD (Figure 3). Attempts were made
to harness and extract the worm(s) with a Dormia basket or
‘rat-tooth’ forceps. Failing the above, an endoscopic balloon
was employed to extract the worm out of the CBD and once
outside the papilla, the worm was grasped with the forceps
and extracted successfully. We made sure to deliver all the
worms, whether in the bile duct or the duodenum, by
withdrawing the endoscope completely and avert any chance
of their re-entry. Endoscopic extraction of the worm(s) was
successful in all patients. The patients were subsequently
administered albendazole 400 mg daily for three days and
mebendazole 200 mg twice daily for three days. After discharge
patients were advised to take albendazole 400 mg once every
three months. Over a median follow-up of 2 yrs (2 wks - 4 yrs)
one patient returned after eight months with recurrence of
symptoms. On ultrasound examination she was detected to have round worm re-infestation in her CBD and was confirmed
on ERCP and the worm was successfully removed in the same
manner as before. Rest of the patients continue to be
asymptomatic.
Discussion
In the present report seven out of nine patients were females.
A higher prevalence in the female sex has been documented by
several other reports as well.[1,4,8] This has been attributed to
progesterone induced sphincter of Oddi relaxation promoting
migration of worm into the biliary tree.[4] In another report prior
sphincterotomy has been attributed as the major cause for
biliary ascariasis.[5] In our experience four patients had prior
endoscopic sphincterotomy and one had biliary bypass in the
form of choledochoduodenostomy. Thus, sphincter ablation
emerged as the most important cause in our cohort prompting
migration of the worms into the biliary tree.
Pain is the commonest mode of presentation in biliary
ascariasis and has been reported in 60-90% patients across
various series.[1,2,3,4,8] Though described as biliary colic in these
reports, the round worm induced pain in our experience was
quite typical and merits further qualification. All but one patient
presented with acute onset pain abdomen that mimicked
pancreatic pain i.e. acute upper abdominal pain radiating to the
back, except that it was waxing and waning in nature with minimal
abdominal signs. The serum amylase was normal in these
patients thus excluding pancreatitis as the cause of pain. The
other presenting features of biliary ascariasis are obstructive
jaundice, acute cholangitis, acute cholecystitis, acute
pancreatitis and liver abscess.[1,2,3,4,8] Only one patient in our study
presented with acute cholecystitis. None of our patients
showed any clinical or biochemical evidence of biliary
obstruction. This is pertinent since majority of our patients
had prior sphincterotomy that did not allow complete
obstruction to occur. In addition the movement of a live worm
in and out of the CBD resulting in an intermittent obstruction
is a well known phenomenon.
Ultrasound examination of abdomen is a reliable screening
tool for the diagnosis of biliary ascariasis.[7,9] In our series the
presence of round worm in the biliary tree could be detected in
all the eight patients who underwent this ultrasound
examination. On endoscopy, a worm projecting out of the papilla
was noted in one of our patients and offered a definitive
confirmation of the diagnosis. On ERC linear or curvilinear
filling defects in the biliary tree confirm ultrasound findings
and the diagnosis of biliary ascariasis. However in cases with
positive ultrasound findings but lack of a filling defect in the
cholangiogram the diagnosis may be explained by the presence
of a live worm in the vicinity of papilla since they are known to
move back and forth in the CBD.
Conservative treatment and oral antihelminthics have been
found to be successful in more than 80% of patients with biliary
ascariasis.[2,10,11] Some authors, however, recommend early
intervention to ward off complications.[1,3,8] Surgical intervention
can be undertaken in the form of cholecystectomy and/or CBD
exploration with complete removal of the worms.[2,3]
Synchronous enterotomy and worm extraction has also been
performed to ward off re-infection. When facilities are available
endoscopic extraction of the worms appear to be a better
alternative and gives prompt relief.[1,4,5,8,9] Endoscopic extraction
was successful in all our patients and provided a prompt relief
to the agonizing pain they were suffering from. Re-infection
was noted in one of our patients. This is similar to the
experience reported by other authors.[12] To minimize the problem of recurrence, they recommend endoscopic balloon
sphincteroplasty instead of conventional sphincterotomy prior
to worm extraction from CBD. Though we concur with the
authors on this issue, we did not have the opportunity to employ
this in our patients.
Conclusion
Biliary ascariasis, though uncommon in non-endemic area,
should be considered in the diagnosis of acute abdomen. This
is particularly true in patients who have undergone prior biliary
sphincter ablation/ bypass procedures like sphincterotomy or
choledochoduodenostomy. Pain could be the only presenting
feature and is often out of proportions to the abdominal signs.
Ultrasound is a reliable screening test for diagnosis and ERC
provides confirmation. Once diagnosed, endoscopic extraction
of the worm is often successful and provides prompt relief to
the patient. Antihelminthics should be administered for
eradication of worms from the intestine and to prevent their reentry
into the biliary tree.
References
- Khuroo MS, Zargar SA, Mahajan R. Hepatobiliary and pancreatic ascariasis in India. Lancet. 1990;335:1503–6.
- Wani NA, Chrungoo RK. Biliary ascariasis: Surgical aspects. World J Surg. 1992;16:976–9.
- Wani MY, Chechak BA, Reshi F, Pandita S, Rather MH, Sheikh TA, et al.Our experience of biliaary ascariasis in children. J Indian Assoc Pediatr Surg. 2006;11:129–32.
- Misra SP, Dwivedi M. Clinical features and management of biliary ascariasis in a non-endemic area. Postgrad Med J. 2000;76:29–32.
- Gupta R, Agarwal DK, Choudhuri GD, Saraswat VA, Baijal SS.
Biliary ascariasis complicating endoscopic sphincterotomy for choledocholithiasis in India. J Gastroenterol Hepatol. 2008;13:1072–3.
- Pilankar KS, Amarapurkar AD, Joshi RM, Shetty TS, Khithani AS, Chemburkar VV. Hepatololithiasis with biliary ascariasis— a case report. BMC Gastroenterology. 2003;3:35.
- Garg A, Hanchate V, Chawla S, Sangle P . Biliary ascariasis. Appl Radiol. 2002;31:33–5.
- Alam S, Mustafa G, Ahmad N, Khan M. Presentation and endoscopic management of biliary ascariasis. Southeast Asian J Trop Med Public Health. 2007;38:631–5.
- Khuroo MS, Zargar SA. Biliary ascariasis. A common cause of biliary and pancreatic disease in an endemic area. Gastroenterology. 1985;88:418–23.
- Louw JH. Biliary ascariasis in childhood. S Afr J Surg. 1974;12:219–25.
- Lloyd DA. Massive hepatobiliary ascariasis in childhood. Br J Surg. 1981;68:468–73.
- Misra SP, Dwivedi M. Removal of Ascaris lumbricoides from the bile duct using balloon sphincteroplasty. Endoscopy. 1998;30:S6–7.