Evangelos Falidas, Emmanouil Pavlakis, Stavros Mathioulakis, Konstantinos Vlachos, Constantinos Villias
1st Department of General Surgery,
417 NIMTS, Veterans Hospital of Athens,
Monis Petraki 10-12,
Athens, 11521, Greece
Corresponding Author:
Evangelos Falidas,
Email: falidase@otenet.gr
48uep6bbphidvals|565 48uep6bbph|2000F98CTab_Articles|Fulltext Villous adenomatous polyps of the colon represent a real potential for cancer development[1]. They also may be involved in abnormal secretory activity associated with diarrhea and electrolyte imbalance, rectal bleeding or obstruction [2,3]. Association between giant villous adenomas (carpet-like lesion) and rectal prolapse is uncommon [4,5]. We present a case of an 87 year old man presented to the emergency department because of an incarcerated rectal prolapse totally carpeted by a giant villous rectal adenoma.
Case presentation
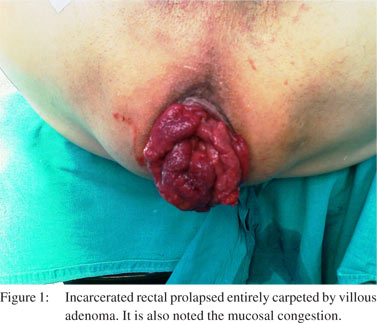
An 87 year old man arrived to the emergency department because of incarcerated rectal prolapse of 6 hours duration. The patient had a history of obstructive airway disease , treated with salmeterol and fluticasone (50+250 mcg, inhalation twice daily) and ipratropium 40mcg (inhalation, three times daily). He had a rectal prolapse diagnosed 5 years ago by a general practitioner, although, he always refused further colonoscopic evaluation or surgical treatment since the rectal prolapse wasreducted spontaneously. Six months prior to presentation, the rectal prolapse needed a manual replacement after defecation. On admission, he did not refer abdominal pain, bleeding or diarrhea. He only mentioned chronic constipation and rarely urgency of defecation. Physical examination did not reveal abdominal pain or signs of intestinal obstruction. Rectal inspection revealed a sizable prolapse entirely carpeted by a large polypoid lesion (Figure 1). Mucosal congestion was also observed while ischemic alterations were limited. Manual reduction was unsuccessfully attempted. Abnormal laboratory findings included mild hypokalhemia (3,2 mg/dl) and hyponatremia (130 mg/dl).
A minimal mobilization and reduction was obtained under general anesthesia, however, a considerable part of the rectum and the associated neoplastic lesion was still protruding through the anus. We initially considered the aspect and the size of the neoplastic lesion regarding possible cancer degeneration, however, we excluded an operation that could combine oncologic benefits and simultaneously, repair of the incarcerated rectal prolapsed. We finally performed a perineal recto-sigmoidectomy (Altemeier’s procedure). The postoperative course was uneventful. He was discharged 7 days later. The pathology report described a large villous adenoma occupying the entire circumference of the resected segment with signs of moderate dysplasia. Colonoscopy was performed 2 months later and no signs of recurrence or of additional colonic neoplasms were observed. No incontinence was observed during a 12 months follow-up.
Discussion
Villous adenomas compromise approximately 10% of all colonic adenomas [1]. Villous adenomas are considered premalignant lesions and usually affect patients over the 5th decade of life [1]. They may be asymptomatic or related with mucus excretion, diarrhea, electrolyte imbalance (Mackittrick-Weelock syndrome), bleeding or obstruction [2,3]. Malignant behavior of these lesions is related with the size. Polyps over 2cm in diameter present a higher risk of malignant degeneration [6]. Carpet-like lesions were first described by Rubesin et al. with double contrast barium enema. They may involve the entire circumference of colonic segment with minimal or not protrusion into the lumen and may occur everywhere into the colon [7]. Some times these lesions may be totally indistinguishable from the normal surrounding colonic mucosa on colonoscopy. The prevalence of carpet lesion has not been well described [8]. Colonoscopy may only describe the lesion while biopsies taken are not always indicative of the malignant status of the mass, given its large surface. On the other hand, rectal prolapse is a full thickness protrusion of the rectum through the anal canal sphincter mechanism. Rectal prolapse carpeted by giant villous adenoma have rarely been reported [4,5]. In addition, rectal prolapse is favored by constipation and other conditions of increased intrabdominal pressure. Some authors observed increased incidence of rectal cancer in patients with untreated chronic rectal prolapse probably due to changes in bowel habits, chronic constipation and chronic irritation[9]. Others consider that rectal prolapse could be attributed to chronic constipation exacerbated by colorectal cancer and for that reason rectal prolapse should be considered a symptom of colorectal neoplasm[10].
Altemeier’s procedure is a valid surgical option in cases of older patients with rectal prolapse associated with sizable carpeted polypoid lesions of the rectum.
References
- Teoh SK., Whitman GJ, Chew FS. Villous adenoma of the colon. AJR. 1996;167:1146
- Mc-Kittrick LS, Wheelock FC Jr. Carcinoma of the colon. Springfield, III: Charles C Thomas, 1954:61
- Jatzko G, Siebert F, Wolf B, Karner-Hanusch J, Kleinert R, Denk H. (1999) Combined restorative proctocolectomy and pancreaticoduodenectomy for familial adenomatous polyposis. Z Gastroenterol. 1999;37:1109–13.
- Shah PR, Joseph A, Haray PN, Kiberu S. Giant villous adenoma in an incarcerated rectal prolapse: a clinical conundrum! Indian J Surg. 2005;67:100–101
- Pinto AC, Desa LA, Pyasi RR, D’Sousa FH. Giant tubulovillous adenoma of rectum presenting as rectal prolapsed. Bombay Hospital Journal. 2008;50:646–7
- Muto T, Bussey HJ, Morson BC. The evolution of cancer of the colon and rectum. Cancer. 1975;36: 2251–70
- Rubesin SE, Saul SH, Laufer I, Levine MS. Carpet lesions of the colon. Radiographics. 1985;5:537–52
- Farag M, Salkani AP, Naguib N, Masoud AG. The red rectum (Carpet villous adenoma of the rectum). JSCR. 2010;10:10
- Lisa KJ, Lin YJ, Orkun BA. The best operation for rectal prolapse. Surg Clin North America. 1997;77:49–70
- Rashid Z, Basson MD. Association of rectal prolapse with colorectal cancer. Surgery. 1996;119:51–5
|