48uep6bbphidvals|506
48uep6bbph|2000F98CTab_Articles|Fulltext
Infestation with Ascaris lumbricoides is a worldwide phenomenon. While most patients with Ascaris infection are asymptomatic, life threatening gastrointestinal conditions may develop that require immediate medical and surgical intervention.[1] This report documents a case of perforation with gangrene of the intestine in a 25 year old male.
Case report
A 25-year-old male presented to the emergency with three day history of epigastric pain associated with nausea, anorexia and vomiting. The patient was febrile and tachypneic on examination. Abdominal examination revealed a hugely distended abdomen and board-like rigidity on palpation. There was generalized tenderness with rebound tenderness. Bowel sounds were absent.
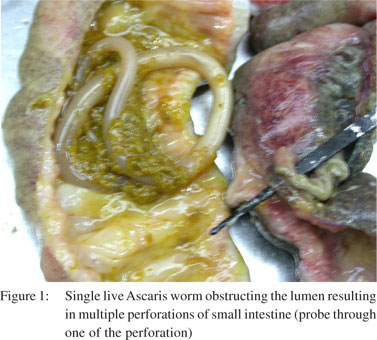
An abdominal radiograph taken in the supine and erect positions showed air under the diaphragm with several airfluid interfaces and free air in the abdomen. With a clinical diagnosis of acute abdomen due to hollow viscus perforation, an exploratory laparotomy was performed. Per-operatively, distal jejunum was found gangrenous with multiple perforations. Resection and anastomosis was performed and specimen was sent for histopathology. Gross examination showed serosal exudates with ulceration of mucosa and an Ascaris worm in the lumen (Figure 1). Microscopy showed mucosal gangrene with submucosal inflammatory infiltrate. A final diagnosis of jejunal gangrene with perforation due to ascariasis was made. Post-operatively, the patient received a course of mebendazole and is asymptomatic over one year follow-up period.
 Discussion
The commonest complication of ascariasis is intestinal obstruction due to a worm bolus.[2] The obstruction may be acute or subacute. It can be complicated by intussusception, perforation and gangrene of the bowel. In ascariasis, the cause of perforation of the small intestine remains controversial, with two main theories. In the tropics patients consistently have histories of diseases associated with ulceration of the intestines such as typhoid enteritis, tuberculosis and amebiasis. During extreme conditions, such as inflammation, starvation or worm bolus obstruction, some parasites are believed to migrate into the ulcers and cause perforations.[2] Another possible explanation is that the large worm bolus can lead to pressure necrosis and gangrene.[3] The diseased bowel thus becomes susceptible to rupture by the burrowing action of the worm.[4] Intestinal obstruction and gangrene constitute the most common surgical complications of ascariasis. The mechanism of obstruction is occlusion of the intestinal lumen by worms packed in the distal ileum as well as localized volvulus of a segment of terminal ileum owing to the weight of the roundworms inside. The mechanism of gangrene may be due to pressure necrosis caused by the roundworms and the accompanying localized volvulus. In patients with ascariasis who present with acute surgical conditions, an urgent laparotomy is indicated to deal with intestinal perforation, to control peritonitis and to decompress the worm bolus that may be causing the acute intestinal obstruction.[1] In endemic areas, mass treatment with mebendazole should be advocated so as to reduce morbidity and although ascariasis is very rare in developed countries, yet clinicians should consider Ascaris infection in the differential diagnosis of acute abdomen, due to current age ease of traveling, and acquired infections in travelers to tropical regions.
References
Discussion
The commonest complication of ascariasis is intestinal obstruction due to a worm bolus.[2] The obstruction may be acute or subacute. It can be complicated by intussusception, perforation and gangrene of the bowel. In ascariasis, the cause of perforation of the small intestine remains controversial, with two main theories. In the tropics patients consistently have histories of diseases associated with ulceration of the intestines such as typhoid enteritis, tuberculosis and amebiasis. During extreme conditions, such as inflammation, starvation or worm bolus obstruction, some parasites are believed to migrate into the ulcers and cause perforations.[2] Another possible explanation is that the large worm bolus can lead to pressure necrosis and gangrene.[3] The diseased bowel thus becomes susceptible to rupture by the burrowing action of the worm.[4] Intestinal obstruction and gangrene constitute the most common surgical complications of ascariasis. The mechanism of obstruction is occlusion of the intestinal lumen by worms packed in the distal ileum as well as localized volvulus of a segment of terminal ileum owing to the weight of the roundworms inside. The mechanism of gangrene may be due to pressure necrosis caused by the roundworms and the accompanying localized volvulus. In patients with ascariasis who present with acute surgical conditions, an urgent laparotomy is indicated to deal with intestinal perforation, to control peritonitis and to decompress the worm bolus that may be causing the acute intestinal obstruction.[1] In endemic areas, mass treatment with mebendazole should be advocated so as to reduce morbidity and although ascariasis is very rare in developed countries, yet clinicians should consider Ascaris infection in the differential diagnosis of acute abdomen, due to current age ease of traveling, and acquired infections in travelers to tropical regions.
References
- Sridhar VB, Peter JH: Acute Gl and Surgical complications of Ascaris lumbricoides infection. Infect Med 2003; 20:154–9
- Efem SE. Ascaris lumbricoides and intestinal perforation. Br J Surg. 1987;74:643–4.
- Surendran N, Paulose MO. Intestinal complications of round worms in children. J Pediatr Surg.1988;23:931–5.
- Khuroo MS. Ascariasis. Gastroenterol Clin North Am.1996;25:553–77.