Vitamin B 12 also called as cobalamin is a water-soluble vitamin, synthesized by microorganisms and is primarily derived from foods of animal origin. Cobalamin deficiency affects all the organ systems but most commonly affects nervous and hematological systems. The most common cause of vitamin B 12 deficiency worldwide is pernicious anemia.1 However in India it could be related to lack of balanced diet or predominance of vegetarian food habits.2 Vitamin B 12 deficiency can also lead to entero-cytopathy which can manifest as chronic diarrhea and malabsorption. But it is unusual for vitamin B 12 deficiency to present as acute diarrhea with severe dehydration. Our two index cases highlight this rare presentation.
Case Reports
Case 1
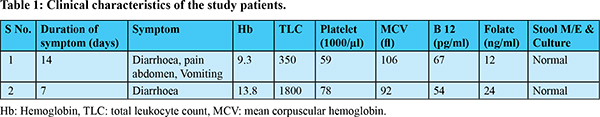
63-year-old male presented with pain abdomen, vomiting and loose stools for last two weeks with marked worsening for the last four days. At admission patient was in hypotension with reduced urine output, and rest of clinical examination was unremarkable. He was started on intravenous (IV) fluid and oral rehydration. Investigations revealed (Table 1): Hb 9.3 g/dl, MCV-106fl (83-101), MCH 37.3 pg (23-32), MCHC 35.2 g/dl (30-35), RDW- 18.3% (10-16), reticulocyte count-0.6%, TLC-350/µl, platelet count 59000/µl, absolute neutrophil count 160/µl, serum (S) creatinine- 1.4 mg/dl, calcium-7.3 mg/dl, phosphorous-1.4 mg/dl, protein- 5.4 g/dl, albumin-2.6 gm/dl, urine routine - protein 2+, Pus cells- 4-5/HPF, RBC- 8-10/HPF, normal liver function tests (LFT), S. sodium-133mEq/L, S. potassium 3.2mEq/L, S. iron- 7µg/dl (70-180), TIBC- 146 µg/dl (250-425), ferritin 519 ng/ml (22-322), normal S. amylase & lipase, normal chest X ray, negative serology for malaria, dengue, scrub typhus, leptospirosis, typhoid, hepatitis B, hepatitis C, HIV, normal stool routine, microscopy, hanging drop & culture, sterile blood & urine culture, vitamin D-10 ng/ml (30-80), serum folate- 12 ng/ml (3.8-26.8), normal IgA TTG, TSH- 3.15 µIU/ml, negative hemolytic work-up, and USG abdomen showing diffuse thickening of small bowel wall with mucosal edema. Patient was managed with IV and oral hydration. But despite hydration and empirical antibiotics, patient continued to have pain abdomen and copious diarrhea. On day 4 of admission,vitamin B 12 level report arrived with value of 67 pg/ml (211-911). So patient was started on IV B 12 (cyanocobalamin) 1000 µg/day, which led to dramatic improvement in the symptoms over next 1-2 days with complete recovery of gastrointestinal (GI) symptoms in 2-3 days. Vitamin B 12 was administered once a day for 6 days followed by once per week for 6 weeks. On follow up at one month patient’s investigations showed HB 13 gm/dl, TLC 5100/µl platelet count 1.26 lakh/µl and CECT abdomen didn’t reveal any abnormality.
Case 2
30-year-old male presented with watery diarrhea, 10-15 episode per day for 7 days. On evaluation patient had severe dehydration, and rest of clinical examination was non-contributory. Patient was started on IV and oral hydration and empirical antibiotics. Investigations revealed (Table 1): Hb-13.8 g/dl, TLC-1800/µl, platelet count-78000/µl, MCV- 92 fl, RDW 15.1% (10-16), MCH-33.2 pg, MCHC- 35.9 g/dl, reticulocyte count- 0.1%, S. sodium- 125 mEq/L, S. potassium- 3mEq/L, uric acid- 9.2 mg/dl, maximum S. creatinine- 9.6 mg/dl, calcium- 8.9 g/dl, phosphorous- 5.5 g/dl, SGOT-159 U/L, SGPT- 52 U/L, protein- 5.1 g/dl, albumin 2.4 g/dl, Stool routine, microscopy, hanging drop, culture-normal, serum folate- 24 ng/ml (3.8-26.8), urine- protein 1+, Pus cells- 2-3/HPF, RBC- 4-5/HPF, negative hemolytic work up, sterile blood & urine culture, normal chest X ray, negative serology for leptospirosis, malaria, dengue, scrub typhus, typhoid, hepatitis B, hepatitis C, HIV, and normal USG abdomen. Despite adequate hydration patient didn’t have any relief of diarrhea and progressed to oligo-anuria. Patient received 4 sessions of hemodialysis. Once low vitamin B 12 level (54 pg/ml) report arrived, patient was started on IV B 12 1000 µg once daily with gradual improvement in GI symptoms over period of 4-5 days. With resolution of diarrhea, urine output began to improve and patient’s dialysis was gradually tapered off. Vitamin B 12 was administered once a day for 6 days followed by once per week for 6 weeks. On follow up at one month patient was asymptomatic and investigations showed HB of 14.5 gm/dl, TLC 8900/µl, platelet count 1.55 lakh/µl, and S. creatinine 1.16 mg/dl.
Discussion
These two cases highlight that acute life-threatening diarrhoea could be the sole initial presenting feature of vitamin B 12 deficiency. In our first case, presence of macrocytic anemia with pancytopenia led us to think of vitamin B 12 deficiency. However, our second case didn’t have characteristic macrocytic anaemia, but had thrombocytopenia and leucopenia. Current literature mainly envisages that vitamin B 12 deficiency can lead to chronic diarrhea and malabsorption. But acute diarrhoea has been seldom attributed to vitamin B 12 deficiency. In our patients acute life-threatening diarrhoea was the sole presenting symptom of vitamin B 12 deficiency. Interestingly in our patients treatment with vitamin B 12 led to rapid recovery from diarrhea and gradual resolution of hematological manifestations, which gives strong credence that B 12 deficiency can present with acute diarrhea with severe dehydration. Both of our patients were not taking animal-based food for long time and after clinically excluding other causes of B 12 deficiency, we attribute this vitamin B 12 deficiency in them to be of nutritional origin.
Cobalamin is a B vitamin that has an important role in cellular and mitochondrial metabolism, especially in DNA synthesis and methylation. Although daily requirement of vitamin B 12 is quite small, ranging from 3.8?µg/d to 20.7?µg/d, but still its deficiency is quite common.3,4 Deficiency of cobalamin mainly affects bone marrow and nervous system, but epithelial surfaces of gastrointestinal (GI), urogenital and respiratory systems can also be affected by vitamin B 12 deficiency. If GI system is affected it can present as glossitis, angular cheilosis, anorexia, weight loss, diarrhea, constipation and jaundice(unconjugated hyperbilirubinemia).4,5 Cells lining the GI tract are characterized by their high turnover, and so they have high B 12 requirement. Vitamin B 12 deficiency impairs division and metabolism of enterocytes and so alters the functioning of enteric mucosa, which can manifest as diarrhea and malabsorption. Chronic diarrhea has been commonly reported to be caused by cobalamin deficiency.4,5,6 But acute diarrhoea with life threatening dehydration has been rarely attributed to vitamin B 12 deficiency. Macrocytic anemia is usually the first lead point to consider vitamin B 12 deficiency, but by solely relying on it we can miss a substantial proportion of B 12-deficient individuals. This observation has been highlighted by Carmel, who states that “The proscription that vitamin B 12 deficiency should not be diagnosed unless megaloblastic changes are found is akin to requiring the presence of jaundice to diagnose liver disease”.7
Conclusion
Vitamin B12 deficiency can masquerade as multitude of illnesses. Our case series highlights that acute diarrhea could be one of the presenting features of cobalamin deficiency. Presence of cytopenia and macrocytosis could lead one to think of cobalamin deficiency as a likely cause of acute diarrhea, but should not be the sole criteria. Awareness about cobalamin deficiency associated acute diarrhea can help us in rapid institution of appropriate therapy and prove to be lifesaving.
References
- Stabler SP, Allen RH. Vitamin B12 deficiency as a worldwide problem. Annu Rev Nutr 2004;24:299-326.
- Singla R, Garg A, Surana V, Aggarwal S, Gupta G, Singla S. Vitamin B12 Deficiency is Endemic in Indian Population: A Perspective from North India. Indian J Endocrinol Metab. 2019;23:211-214.
- Doets EL, In ‘t Veld PH, Szczecinska A, Dhonukshe-Rutten RA, Cavelaars AE, van ‘t Veer P, et al. Systematic review on daily vitamin B12 losses and bioavailability for deriving recommendations on vitamin B12 intake with the factorial approach. Ann Nutr Metab. 2013;62:311-22.
- Green R, Allen L, Bjørke-Monsen A, Brito A, Guéant J, Miller J, et al. Vitamin B deficiency. Nat Rev Dis Primers. 2017;3:17040.
- Hoffbrand AV. Megaloblastic anaemias. In: Loscalzo J, Fauci AS, Kasper DL, Hauser SL, Longo DL, Jameson JL, Editor(s). Harrison’s principles of internal medicine. 21sted. New York: McGraw Hill; 2022. p. 766-76.
- Mendonça FM, Leitão MJ, Faria-Costa G, Pires Da Rosa G, Almeida J. Chronic diarrhea: an unusual clinical presentation of vitamin B12 deficiency? Intern Emerg Med. 2019 Apr;14:491-492.
- Carmel R. Current concepts in cobalamin deficiency. Annu Rev Med. 2000; 51:3