Ira Shah 1, Susmita Bhatnagar2
Department of Pediatric Medicine1 and Pediatric Surgery2
Hepatobiliary Clinic, B. J. Wadia Hospital for Children,
Parel, Mumbai-400012
Corresponding Author:
Dr. Ira Shah
Email:irashah@pediatriconcall.com
Abstract
Aim: To determine etiological spectrum as well as clinical profile of chronic hepatobiliary disorders in children.
Methods: 45 children with chronic hepatobiliary disorders were evaluated in the study.out of 105 children with liver diseases referred to the clinic. . All underwent detailed history and clinical examination. Clinical and laboratory features as well as causes of chronic hepatobiliary disorders were studied.
Results:- The common causes were biliary atresia in 11 (25%) patients, neonatal hepatitis and Wilson’s disease in 6 (13%) patients each, glycogen storage disorder (GSD) and idiopathic hepatitis in 5 patients (11%) each, Hepatitis B in 2 (5%), Hepatitis C in 1 (2%), Hepatitis B and C in 1 (2%), Caroli’s disease in 2 (5%), autoimmune hepatitis in 2 (5%); sclerosing cholangitis, viral hemophagocytosis and thalassemia major in 1 (2%) patient each. Common clinical presentations were jaundice in 32 (71%), dark urine in 19 (42%), fever in 13 (29%), failure to thrive in 7 (16%), splenomegaly in 21 (47%) and hepatomegaly in 32 (71%). Also children with neonatal cholestasis presented in 1st year of life, those with idiopathic liver disease and GSD presented within 1st 5 years of life and those with Wilson’s disease. Autoimmune hepatitis, Caroli’s disease presented between 5-10 years of age and viral hepatitis was seen in 2nd decade of life (p <0.001).
Conclusion: - Commonest cause of chronic hepatobiliary disorders in children is neonatal hepatitis. Metabolic liver disease usually presents in 1st 5 years of life whereas chronic viral hepatitis has a presentation in adolescence.
|
48uep6bbphidcol4|ID 48uep6bbphidvals|308 48uep6bbph|2000F98CTab_Articles|Fulltext Chronic liver diseases constitute 36% referral to a pediatric gastroenterology clinic in India [1,2]. The common causes of chronic hepatobiliary disorders have varied from centre to centre with Wilson’s disease and metabolic disorders being commonly reported from Lucknow [1], Indian childhood cirrhosis from Pune [3], infantile cholangiopathy from Delhi [4], Hepatitis B from Karachi [5] in the Indian subcontinent. We, thus, undertook this study to determine common causes of chronic hepatobiliary disorders in Western India and also determine their clinical profile. Our centre is a tertiary referral centre and patients from Western India are referred for specialized treatment.
Methods
All children with suspected chronic hepatobiliary disorders referred to our Pediatric Hepatobiliary clinic were enrolled in the study. They underwent detailed history and thorough clinical examination. Complete blood counts, liver function tests and ultrasound of abdomen were done in all patients. To determine the etiology of chronic liver disease, viral markers including HBsAg and Anti HCV, markers for autoimmune disease [antinuclear antibody (ANA), anti smooth muscle antibody (Anti SMA) and anti liver-kidneymicrosomal antibody (Anti LKM-1)] and metabolic screening for Wilson’s disease (slit lamp examination for KF ring, hepatic copper content and urinary copper) was done. Chronic hepatobiliary disorders due to neonatal cholestasis syndrome (NCS) was diagnosed as persistence of liver inflammation with history of neonatal cholestasis (conjugated jaundice in first three months of life) and/or Kasai portoenterostomy. Glycogen storage disorder was diagnosed by presence of glycogen on liver biopsy. Caroli’s disease was diagnosed by presence of biliary cysts and co-existing polycystic kidney disease. Hemophagocytic syndrome was diagnosed by fever, hepatic failure, pancytopenia and bone marrow demonstrating hemophagocytes.
In addition, majority of patients were subjected to liver biopsy. Alpha-1 antitrypsin levels were done in selected patients. Urine aminoacidogram (UAA) was done to rule out Tyrosinemia. All patients were treated with multivitamins and specific agents for their respective cause of liver disease. Clinical and biochemical factors of chronic hepatobiliary disorders and their association with various etiologies of CLD were analyzed.
Statistical Analysis: - The clinical manifestations and laboratory findings of each type of disease were compared using chi-square or fisher’s exact test for proportions and analysis of variance (ANOVA – 1 way) for continuous data.
Results
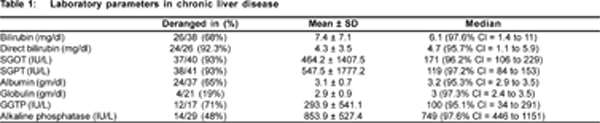
45 children with chronic hepatobiliary disorders were evaluated. The mean age of presentation was 4.1 ± 3.9 years with median of 3 years and range of 3 months to 13 years. Male: Female ratio was 27:17 (in 1 patient, data was missing). The common clinical features were jaundice in 32 (71%), dark urine in 19 (.42%), fever in 13 (29%), failure to thrive in 7 (16%), splenomegaly in 21 (47%) and hepatomegaly in 32 (71%). Ascites was present in 3 patients who had fulminant hepatic failure and all 3 of them died. The average number of days of jaundice was 326.7 ± 599.2 days with median of 60 days and range from 4 days to 7 years. The median days of fever was 14 days (97.8% Cl = 5 to 30 days) and median days of high coloured urine was 60 days (96.9% Cl = 8 to 135 days). The laboratory parameters are depicted in Table 1.
The various causes of chronic hepatobiliary disorders are neonatal cholestasis syndrome in 17 (38%) patients of which 11 had biliary atresia, Wilson’s disease in 6 (13%), Glycogen storage disease in 5 (11%), Hepatitis B in 2 (5%), Autoimmune hepatitis in 2 (5%), Caroli’s disease in 2 (5%), Sclerosing cholangitis in 1 (2%), hemophagocytosis in 1 (2%), Hepatitis C infection in 1 (2%), mixed Hepatitis B & C in 1 (2%) and thalassemia major in 1 (2%) patient.
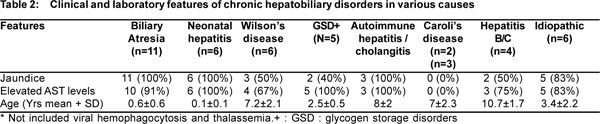
No etiology was found in 6 (13%) patients. The various clinical and laboratory parameters associated with different causes of CLD are depicted in Table 2.
Ten patients had cirrhosis (22%). On follow-up, 27 (60%) patients were on regular treatment, 15 (33%) were lost to follow-up and 3 patients (7%) died of fulminant hepatic failure of which one had glycogen storage disease, the other had viral hemophagocytic syndrome and patient with sclerosing cholangitis died due to hepatocellular failure. Eight patients had portal hypertension on colour Doppler. Liver biopsy was done in 36 patients and showed cirrhosis in 10 patients.
Discussion
The commonest cause of chronic hepatobiliary disorders at our centre is neonatal hepatitis and biliary atresia which makes up almost 38% of the referrals. This is unlike that reported from other centres where metabolic disorders, viral hepatitis and Indian childhood cirrhosis have been reported as common causes of chronic liver diseases (CLD).[1,3,5] A study from Eastern India has reported Hepatitis B and C, Wilson’s disease, autoimmunity and alcohol as common causes of CLD in adults [6]. Thus, causes of CLD in children tend to vary from centre to centre and are not uniform throughout requiring detailed analysis of each patient referred. Other causes of CLD in our patients were metabolic such as Wilson’s disease, storage disorders such as glycogen storage disorder, autoimmune hepatitis, Hepatitis B and C and Caroli’s disease. Rare causes were viral hemophagocytosis and thalassemia. Other disorders such as Alpha-1-antitrypsin and Indian childhood cirrhosis were not seen at our centre.
Common clinical presentations reported earlier have been edema, jaundice, variceal bleeding, fever, anemia, splenomegaly, hypoalbuminemia, hepatomegaly.[4,5] In our study, common presentations of chronic hepatobiliary disorders were jaundice, hepatomegaly, splenomegaly, elevated serum transaminases (upto 10 times elevated) with hypoalbuminemia (mean serum albumin = 3.1 gm/dl) and fever. Fulminant hepatic failure was a presentation in 3 children and all of them died. Similarly Yachha et al found that fulminant hepatic failure was the presentation in 4% of children with liver disease.[1]
However, in our study we found that in patients with neonatal cholestasis, autoimmune hepatitis and idiopathic liver disease; jaundice is a predominant feature whereas in 50% of patients with Wilson’s disease, GSD and viral hepatitis, jaundice may not be the presenting feature. Also patients with Caroli’s disease presented without jaundice and predominantly only as hepatosplenomegaly. Though elevated liver transaminanses are seen in most children, AST remains normal in Caroli’s disease (p = 0.03). It was also seen that the age of presentation tends to vary with neonatal cholestasis presenting in infancy; GSD and idiopathic hepatitis presenting in children less than 5 years of age and Wilson’s disease, autoimmune hepatitis, chronic viral hepatitis and Caroli’s disease presenting in older children. Similar age related manifestation have not been reported earlier [1,2,3]
In conclusion the commonest causes of chronic hepatiobiliary disorders in pediatric age group were biliary atresia and neonatal cholestatsis in a tertiary referral centre in Western India.
References
1. Yachha SK, Sharma BC, Khanduri A, Srivastava A. Current spectrum of hepatobiliary disorders in northern India. Indian Pediatr. 1997;34:885–90.
2. Bhave SA, Bavdekar A, Pandit AN. Changing pattern of chronic liver disease (CLD) in India. Indian J Pediatr. 1994;61:675–82.
3. Bhave SA, Pandit AN, Pradhan AM, Sidhaye DG, Kantarjian A, Williams A, et al. Liver disease in India. Arch Dis Child. 1982;57:922–8.
4. Dangwal TR, Aggarwal V, Malhotra V, Baveja U, Mittal SK. Clinical spectrum of chronic liver disease in north Indian children. Trop Gastroenterol. 1997;18:174–6.
5. Hanif M, Raza J, Qureshi H, Issani Z. Etiology of chronic liver disease in children. JPMA. 2004;54:119–22.
6. Ray G, Ghoshal UC, Banerjee PK, Pal BB, Dhar K, Pal AK, et al. Aetiological spectrum of chronic liver disease in eastern India. Trop Gastroenterol. 2000;21:60–62.
|