48uep6bbphidvals|253
48uep6bbphidcol4|ID
48uep6bbph|2000F98CTab_Articles|Fulltext
Salmonella typhi infection is well known to affect the gall bladder and cause acalculus cholecystitis. A large distended gall bladder may then develop areas of necrosis and perforate. Perforation of a typhoid gall bladder, though known, is a rare entity.
Case report
A 14-year-old girl presented to surgery emergency with a 15- day history of high grade fever and generalized pain abdomen for 10 days. The pain was associated with progressive distention of abdomen and non-passage of flatus and feces for two days. On examination, the patient was hemodynamically stable. There was generalized abdominal tenderness, guarding and rigidity, and free fluid in the abdomen. Widal test, performed three days prior to admission, was positive for Salmonella typhi ‘O’ and ‘H’ in 1:320 dilution and for Salmonella paratyphi ‘AH’ in 1:160 dilution. Hematological investigations at the time of admission revealed anemia with hemoglobin level of 7.7gm/ dl and total leukocyte count of 8700/mm3. Plain X ray of the abdomen (erect view) did not show pneumoperitoneum. Ultrasonography (USG) of the abdomen showed free fluid in the abdomen with normal liver, the gall bladder was not visualized.
A provisional diagnosis of typhoid ileal perforation was made and an exploratory laparotomy was performed. During operation, about 1 liter of bilious fluid was found in the peritoneal cavity. The whole of the gall bladder was congested, with two perforations in the gall bladder wall near the infundibulum. No stone was palpable in the gall bladder, or common bile duct. No stone was found lying free in the peritoneal cavity. Cholecystectomy was performed and thorough peritoneal lavage was undertaken. Abdomen was closed after placing tube drains in the right sub hepatic space and pelvis. Injection ceftriaxone and gentamicin was administered post operatively. The patient made an uneventful recovery and was discharged on the seventh postoperative day. Histopathological examination of the resected gall bladder showed aggregates of lymphoid follicles in the mucosa with mononuclear infiltrate and erythrophagocytosis, suggesting enteric etiology (Figure 1 and 2).
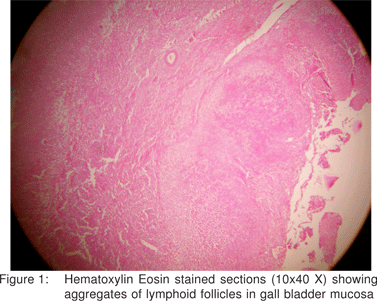
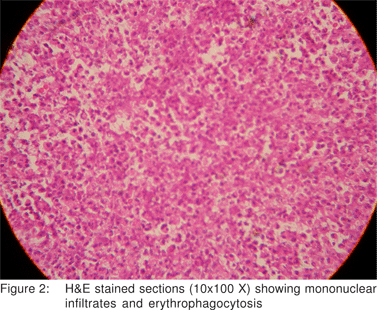
Discussion
Gall bladder is more likely to perforate in cases of obstruction leading to raised intra luminal tension. Non obstructive cholecystitis is unlikely to result in perforation.[1] Perforation complicating acute acalculus cholecystitis is often seen in association with acute infections like pneumonia, viral influenza, and in particular with typhoid where the causative organism Salmonella typhii multiply in bile in very high titers and are further concentrated in gall bladder[2]. Perforation in such cases is likely to be caused by intense inflammation coupled with infection with more virulent organisms and existence of a immuno compromised state leading to thrombosis of the blood vessels. This in turn causes transmural necrosis and perforation. Younger patients in an immuno compromised state also have a higher incidence of perforation[3]. Gall bladder perforations due to typhoid fever, though known, have been rarely reported over the past two decades[3,4,5]. Most of the reported cases of enteric gall bladder perforation date back to 1970s.
Peritonitis due to gall bladder perforation is associated with high mortality as quoted by Essenhigh (39.1%)1. This high mortality makes timely diagnosis and management of perforated gall bladder highly crucial. Diagnostic peritoneal lavage in gall ladder perforation yields bile with or without blood. However, the presence of bile indicates biliary tract injury and is not specific for gall bladder perforation.
USG is useful in 70% of cases in diagnosing gall bladder perforation and detecting the defect in gall bladder wall and hence it can be used as first line imaging modality for evaluating such a case[6]. The features of non–traumatic gall bladder perforation on USG are free fluid and fluid collections close to the gall bladder fossa, thickened gall bladder wall – 7 mm (range 3-20 mm) and localized collection in gall bladder wall. CT scan shows free fluid and localized perihepatic and gall bladder fossa collections. The gall bladder can be accurately identified and the site of perforation is often demonstrated.
Perforation of the gall bladder must be treated surgically when the diagnosis is made or suspected. The preferred procedure is emergency cholecystectomy. Cholecystostomy is an acceptable alternative especially in poor risk patients.
References
1. Essenhigh DM. Perforation of the gall-bladder. Br J Surg. 1968;55:175–8.
2. Christie AB. Typhoid and paratyphoid fever. In Christie AB, editor. Infectious Diseases: Epidemiology and Clinical Practice. 3rd ed. New York: Churchill Livingstone; 1980. p. 47.
3. Kamble AT, Sarda DK, Chaudhary N, Hatwar S. Gall bladder perforation in typhoid fever. J Indian Assoc Pediatr Surg. 2003;8:249–50.
4. Memon AA. Perforated gall bladder A Case Report. J Surg Pakistan. 2001;6:37.
5. Saxena V, Basu S, Sharma CL. Perforation of the gall bladder following typhoid fever- induced ileal perforation. Hong Kong Med J. 2007;13: 475–7.
6. Sood BP, Kalra N, Gupta S, Sidhu R, Gulati M, Khandelwal N, et al. Role of sonography in the diagnosis of gall bladder perforation. J Clin Ultrasound. 2002;30:270–4.