|
RY Prabhu, R Irpatgire, B Naranje, CV Kantharia, RD Bapat, AN Supe
Department of Surgical Gastroenterology
Seth GS Medical College & KEM Hospital,
Parel, Mumbai.
Corresponding Author:
Dr RY Prabhu
Email: drpram4@yahoo.co.in
Abstract
Aim: Gallstone disease is the most common cause of acute pancreatitis. Cholecystectomy is mandatory to avoid recurrence of pancreatitis. Our objective was to evaluate the results of laparoscopic cholecystectomy (LC) in patients with gall-stone induced pancreatitis.
Methods: All patients presenting to us within the time frame from February 2004 to June 2008 with acute biliary pancreatitis were included in the study. The severity of pancreatitis was assessed by Ranson’s criteria. ERCP and endoscopic sphincterotomy was performed when the common bile duct (CBD) was dilated (>6 mm) with either calculi or sludge as seen on imaging. Patients with successful ERCP with predicted demanding laparoscopic cholecystectomy were discharged instead for an elective LC, 4-6 weeks later. Patients with mild pancreatitis (with Ranson’s score of 3 or less) and predicted uncomplicated LC underwent surgery at the same admission. The difficulty of the procedure was determined by the presence of adhesions in the gallbladder area, dissection in Calot’s triangle, tackling the dilated cystic duct, intra-operative bleeding, and the need for a drain.
Results: A total of 26 patients (12 male and 14 female; age range 23-75 years) with acute biliary pancreatitis comprised the study group. Eleven patients with suspected choledocholithiasis underwent ERCP and clearance of the CBD was done in all of them. Nine patients (2 ERCP and 7 non-ERCP) underwent early LC in the same admission. Seventeen patients (9 ERCP and 8 non-ERCP) were predicted as difficult cases for LC and underwent delayed LC. No patient had recurrent pancreatitis in the interval period. Conclusion: There was no significant difference in the operative difficulty between early and delayed LC when patients were selected for timing of LC based on pre-defined criteria.
|
48uep6bbphidvals|243 48uep6bbphidcol2|ID 48uep6bbph|2000F98CTab_Articles|Fulltext Gallstone disease is the commonest cause of acute pancreatitis. In these cases cholecystectomy is absolutely necessary to avoid recurrence of pancreatitis.[1] Laparoscopic cholecystectomy is now the standard procedure for the management of gallbladder stones.[2,3] Some surgeons consider acute biliary pancreatitis a contraindication for laparoscopic cholecystectomy whilst others advocate early surgery, performed shortly after resolution of the pancreatitis.[3,4,5,6] Selective endoscopic retrograde cholangiography (ERC), clearing the bile duct in case of stone and cholecystectomy comprise the current treatment modality in patients with acute biliary pancreatitis (ABP).[7] The advent of biliary decompression with ERC and endoscopic sphincterotomy (ES) allows the surgeon to plan an elective (interval) laparoscopic cholecystectomy for gallstones. There remains a dilemma when choosing between early cholecystectomy to prevent recurrence of pancreatitis and planning interval cholecystectomy to avoid surgery in the acute phase. One of the problems with early cholecystectomy may be the difficultly encountered during surgery due to inflammation and adhesions. Clinical and ultrasonographic features can help predict difficult LC and the likelihood of conversion of LC to open surgery.[8] Our objective was to evaluate the results of laparoscopic cholecystectomy (LC) in patients with gallstone-induced pancreatitis in terms of timing, ease of surgery and results.
Methods
We evaluated all patients presenting to our department between February 2004 and June 2008 with biliary pancreatitis for the study. Acute pancreatitis was defined as acute abdominal pain with elevated serum levels of amylase (40-165 IU/L) and lipase and CRP (0-5 mg/L). To confirm the diagnosis of gallstone pancreatitis all patients were subjected to abdominal ultrasonograpy and magnetic resonance cholangiopancreatography (MRCP) on admission as per protocol (Figure 1).

Patients were included in the study only if there was evidence of gallbladder disease, and where other causes of pancreatitis had been excluded. Patients with previous abdominal surgery were excluded from the study to avoid bias created due to difficulty during laparascopic cholecystectomy. Patients were stratified according to the severity of disease by Ranson’s criteria.
Endoscopic sphincterotomy (ES) and endoscopic retrograde cholangiopancreatography (ERCP) were performed when the common bile duct was dilated with stone(s) demonstrated on imaging studies, along with raised plasma aspartate aminotransferase (AST) more than 60 IU/L, alanine aminotransferase (ALT) more than 150 IU/L.
Clinical improvement was defined as a reduction in the abdominal pain, resumption of feeding and absence of complications. The patient’s clinical profile and USG findings helped predict difficulty for laparoscopic cholecystectomy.
Factors predicting difficult cholecystectomy8 included the following:
1) male patients,
2) body mass index >30 kg/m2,
3) past history of acute cholecystitis,
4) USG findings of gallbladder wall thickness >3 mm,
5) contracted gallbladder,
6) dilated CBD (> 6 mm)
Patients predicted as difficult cases for LC as per the above criteria were discharged for elective interval laparoscopic cholecystectomy 4-6 weeks later and those predicted as easy cases for LC underwent surgery in the same admission regardless of the need and performance of the ERCP (Figure 1). Surgery was performed by experienced laparoscopic surgeons using the standard four ports with additional ports for retraction /dissection whenever required. The cystic duct and cystic artery were separately clipped with Ligal clips (M/s Ethicon Endo Surgery inc.), when the cystic duct was dilated; it was ligated intracorporeally with 2-0 vicryl suture. The gallbladder was extracted through the epigastric port, (in a plastic bag) which was dilated where necessary. The degree of difficulty of the procedure was assessed by the presence of adhesions in the gallbladder area, difficult dissection in Calot’s triangle, intraoperative bleeding, the need for a drain and conversion to an open procedure.
Results
Twenty-six patients with biliary pancreatitis (12 male and 14 female) were included in the study. Their age ranged between 20 and 75 years, (mean 39 years). Thirteen patients had a BMI more than 30 kg/m2. No patient had a history of previous cholecystitis. At admission, 12 patients had scores of less than 3, 9 had 3 and 5 more than 3 on Ranson’s scoring system. A dilated common bile duct (over 6 mm) and suspected choledocholithiasis were found in eleven patients. All patients had increased levels of plasma aspartate aminotransferase (AST) and alanine aminotransferase (ALT). However, only eleven patients who had CBD calculi had significantly increased levels of AST (> 60 IU/L), ALT (>150 IU/L), serum bilirubin and serum alkaline phosphatase. All 11 patients successfully underwent ERCP with endoscopic sphincterotomy, and clearance of stones and sludge from the common duct. There were no complications related to the ERCP. Laparoscopic cholecystectomy was performed in these patients after an interval of 4-6 weeks, to allow the acute inflammation to settle.
Abdominal ultrasonography revealed a thickened gallbladder wall of more than 3 mm in 17 patients and less than 3 mm in 9 patients. A contracted gallbladder was found in seven patients. Nine patients (2 ERCP and 7 non-ERCP) were predicted as easy cases, and underwent early laparoscopic cholecystectomy in the same admission. A total of 17 patients (9 ERCP and 8 non ERCP) were predicted to be difficult cases for laparoscopic cholecystectomy and discharged for interval laparoscopic cholecystectomy. No patient had recurrent pancreatitis in the interval period. Two patients with delayed LC had post cholecystectomy pancreatitis and were managed conservatively.
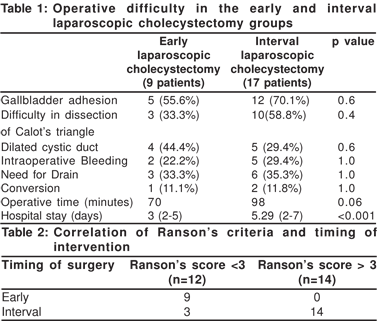
There were no significant differences in the operative difficulty between early and interval laparoscopic cholecystectomy (Table 1). Of 12 patients who had a Ranson’s score <3, 9 underwent early LC and of 14 patients who had Ranson’s score > 3 , none underwent ealy LC (Table 2).
Discussion
Gallstone disease is the most common cause of acute pancreatitis.[1] Most patients with acute biliary pancreatitis suffer a mild attack and are expected to make a full recovery. Cholecystectomy is indicated to prevent recurrence of pancreatitis.[2] Acute biliary pancreatitis was considered a relative contraindication to the laparoscopic approach in the past. However, laparoscopic cholecystectomy with preoperative endoscopic common bile duct clearance if necessary, is currently recommended as the treatment of choice for acute biliary pancreatitis.[1,4,9,10] With the availability of ERCP and ES, the old concept of interval cholecystectomy has regained interest. The wide acceptance of ERCP and ES for urgent decompression of the biliary system enables the surgeon to plan an elective interval cholecystectomy for the residual gallstones and allow the acute inflammation to settle.[11] Though there are reports in the literature of one-third of patients encountering recurrence within an interval of 4-6 weeks which may increase with time,[3,12] there were no recurrent attacks reported during the interval period in the 8 patients in our series who did not undergo ERCP and ES. Although delayed surgery is often advised to allow the inflammation to subside, the results of the present study suggest that delayed laparoscopic cholecystectomy does not offer any benefit over early surgery. This might be explained by the type of patient who was predicted to have difficult LC based on USG findings, male gender and BMI of >30. Another study has also reported similar findings.[8] Predicting difficult LC and conversion to OC may be helpful. A high predicted risk of conversion might allow the surgeon to take an early decision to convert to open cholecystectomy (OC) when difficulty is encountered during dissection; this may shorten the duration of surgery and decrease the associated morbidity.[13]
Conclusion
In conclusion, our results suggest that early cholecystectomy is feasible with less morbidity in patients with nondilated CBD and a Ranson’s score of less than 3; however a wide or dilated cystic duct which may require proper ligation, needs to be kept in mind. Patients predicted to undergo difficult LC based on USG findings, male gender and a BMI greater than 30 should undergo interval LC. There was no significant difference in the operative difficulty between the early and delayed LC when patients were selected for timing of LC based on pre-defined criteria. The lack of statistical difference between the groups might be due to the small sample size in the present study, and thus a larger, possibly multicentric study is required to provide a clear answer.
Acknowledgement
We would like to acknowledge Dr Prriya Eshpuniyani for her contribution in statistical analysis and research for this paper.
References
1. Ricci F, Castaldini G, de Manzoni G, Borzellino G, Rodella L, Kind R. Minimally invasive treatment of acute biliary pancreatitis. Surg Endosc. 1997;11:1179–82.
2. DeIorio AV Jr, Vitale GC, Reynolds M, Larson GM. Acute biliary pancreatitis. The roles of laparoscopic cholecystectomy and endoscopic retrograde cholangiopancreatography. Surg Endosc. 1995;9:392–6.
3. Bismar HA, Al-Salamah SM. Outcome of laparoscopic cholecystectomy in acute biliary pancreatitis. Saudi Med J. 2003;24:660–4.
4. Tate JJ, Lau WY, Li AK. Laparoscopic cholecystectomy for biliary pancreatitis. Br J Surg. 1994;81:720–2.
5. Rosing DK, de Virgilio C, Yaghoubian A, Putnam BA, El Masry M, Kaji A, et al. Early cholecystectomy for mild to moderate gallstone pancreatitis shortens hospital stay. J Am Coll Surg. 2007;205:762–6.
6. Tang E, Stain SC, Tang G, Froes E, Berne TV. Timing of laparoscopic surgery in gallstone pancreatitis. Arch Surg. 1995;130:496–9.
7. Soper NJ, Brunt LM, Callery MP, Edmundowicz SA, Aliperti G. Role of laparoscopic cholecystectomy in the management of acute gallstone pancreatitis. Am J Surg. 1994;167:42–50
8. Nachnani J, Supe A. Pre-operative prediction of difficult laparoscopic cholecystectomy using clinical and ultrasonographic parameters. Indian J Gastroenterol. 2005;24:16–8
9. Bulkin AJ, Tebyani N, Dorazio RA. Gallstone pancreatitis in the era of laparoscopic cholecystectomy. Am Surg. 1997;63:900–3.
10. Uhl W, Müller CA, Krähenbühl L, Schmid SW, Schölzel S, Büchler MW. Acute gallstone pancreatitis: timing of laparoscopic cholecystectomy in mild and severe disease. Surg Endosc. 1999;13:1070–6.
11. Liu CL, Lo CM, Fan ST. Acute biliary pancreatitis: diagnosis and management. World J Surg. 1997;21:149–54.
12. Alimoglu O, Ozkan OV, Sahin M, Akcakaya A, Eryilmaz R, Bas G. Timing of cholecystectomy for acute biliary pancreatitis: outcomes of cholecystectomy on first admission and after recurrent biliary pancreatitis. World J Surg. 2003;27:256–9.
13. Kama NA, Kologlu M, Doganay M, Reis E, Atli M, Dolapci M. A risk score for conversion from laparoscopic to open cholecystectomy. Am J Surg. 2001;181:520–5.
|