48uep6bbphidcol2|ID
48uep6bbphidvals|1898
48uep6bbph|2000F98CTab_Articles|Fulltext
The greater omentum is a long peritoneal foldwhich is in continuity with the visceral fold of peritoneum of stomach as well as transverse colon. It plays a pivotal role in containing the spread of intraperitoneal inflammation. Infarction of the omentum is a rare etiology of acute abdomen with an incidence of approximately 0.3%. Among patients who underwent laparotomies for acute abdomen 0.1% cases were found to have omental infarction.1 It is reported most commonly in the third to fifth decades with male predominance, although person of any age group can be affected by this disorder.1
Case Report
A 52 years old obese male patient without any co-morbidity presented with four months history of heaviness in right lumbar and umbilical region it was insidious in onset and gradually progressive but not associated with abdominal pain. He denied any history of vomiting, diarrhea, constipation, obstipation during his course of illness. Subsequently, patient also noticed a lump in right lower quadrant of abdomen which was progressively increasing. There was no history of trauma to abdomen, fever, jaundice, altered bowel habit, blood in stool, dysuria, hematuria or loss of weight appetite. He had underwent a mesh repair of right sided inguinal hernia two months prior to his admission at our centre. On clinical examination, a lump of 15x15 cm size with distinct borders, smooth surface and firm in consistency was felt on abdominal examination involving the right lumbar, right hypochondrium and right side of umbilical region, and was non tender on palpation. CECT abdomen showed a large mass with predominant fat in the right anterolateral omentum adjacent to the ascending colon with evidence of swirling of a vessel and fat within the mass as (Figure 1). The imaging findings were suggestive of omental infarction resulting from torsion. Esophago-gastro-duodenoscopy and colonoscopy with ileoscopy was normal.
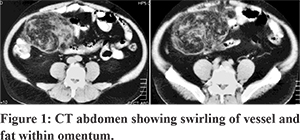
The patient underwent a CT guided FNAC from the abdominal lump that revealed omental fat necrosis with minimal inflammation without any evidence of malignancy or organism which was consistent with the diagnosis of omental infarction (Figure 2). Our patient underwent surgical resection in view of progressive increase in size on follow up CT scan (Figure 3). Histopathology was also consistent with omental infarction without any evidence of malignancy (Figure 4). On follow-up after three month patient was doing well without any fresh complaints.
Discussion
Omental infarction occurs due to compromise of the vasculature mainly involving the greater omentum. Torsion of the omentum has been postulated as the primary mechanism which leads to omental infarction. The basic pathogenesis of omental infarction is due to venous stasis which leads to venous thrombosis, followed by congestion and edema of the peritoneum resulting in hemorrhagic necrosis. This in turn leads to extravasation of serosanguineous fluid into the peritoneum.1 However; its rare occurrence can be explained by the presence of abundant collateral vessels that supply the omentum.2
Primary torsion of the omentum occurs due to a mobile portion of the omentum rotating around a proximally located fixed-point without any associated intra-abdominal pathology. Various predisposing factors like obesity, trauma, hyper-peristalsis, splanchnic ischemia, postprandial congestion of the vasculature, venous kinking due to vigorous activity or coughing and variations in the omental anatomy etc can precipitate omental infarction.1 Right sided torsion is more common due to longer length and greater mobility of the omentum on the right side and hence it is more prone to twisting along its longitudinal axis usually in clockwise direction which compromises the vascularity of the omentum.2
Secondary omental torsion is more common than primary and it occurs in association with pre-existing pathologies in abdomen like intra abdominal inflammations, cysts, tumours, surgical scars, adhesions and presence of hernia sacs.2 Increase in intra-abdominal pressure due to various factors, trauma to abdomen or presence of hernia results in passive displacement and torsion of the omentum.2
Majority of the patients of omental infarction manifests in the form of acute pain in right lower quadrant of abdomen because of the characteristic site of omental infarction which is usually misdiagnosed as acute appendicitis. Rarely left sided omental infarction occurs mainly involving the descending colon which mimics acute diverticulitis, mesenteric panniculitis and epiploic appendagitis in the adult population.2 Some of the patients give history of recurrent pain which suggests intermittent torsion. On clinical examination, half of the patients have abdominal mass at presentation.2 Although our patient has presented with right sided abdominal mass; there was no history of abdominal pain which was quite unusual for omental infarction.
Ultrasound or CECT abdomen is useful diagnostic modality which helps in timely diagnosis of omental infarction as well as selection of cases which can be treated conservatively, optimizing the need for surgery.3,4 Ultrasound abdomen may reveal a complex mass with hyper and hypoechoic areas and presence of ascites. The diagnosis of omental infarction has increased substantially in view of improved awareness about the entity as well as increased use of CT scan for diagnosis of abdominal complaints.
The classical sign of omental torsion which is harbinger of omental infarction on CT scan is the whirl sign, showing a mass which appears fatty with linear strands arranged concentrically in the omentum. These strands represent twisted blood vessels that whirl around a structure located centrally. However, other differential diagnoses like omental hernia, panniculitis, diverticulitis, inflammation of epiploic appendages and fat-containing neoplasms which may present as fatty mass with associated stranding of fat on CT abdomen; need to be considered. MRI is an effective tool when omental infarction is complicated by abscess formation or bleeding.5
The current investigation as well as treatment of choice is laparoscopy followed by laparotomy, where the infarcted section of omentum is identified and then removed.5
Omental infarction is a rare entity which requires a high index of suspicion to diagnose it. In patients presenting with abdominal pain with or without lump after ruling out common causes of abdominal pain, possibility of omental infarction should be considered. Carefully evaluation of CT scan may provide a clue to the diagnosis. Most patients require only conservative treatment. However, if symptomatic or complicated, surgical excision is a treatment of choice.
References
- Breunung N, Strauss P. A diagnostic challenge: primary omental torsion and literature review- a case report. World J Emerg Surg. 2009; 4:40.
- Barbier C, Pradoura JM, Tortuyaux JM. Diagnostic imaging of idiopathic segmental infarct of the greater omentum. Diagnostic and physiopathological considerations. J. Radiol. 1988; 79:1485.
- Wang W, Wang ZJ, Webb EM et al.Omental infarction preceded by anatomically upturned omentum. Clin Imaging. 2013; 37(6):1125–7.
- Tsironis A, Zikos N, Bali C, Pappas-Gogos G, Koulas S, Katsamakis N. Primary Torsion of the Greater Omentum. Report of two cases and Review of the literature. The Internet J Surg. 2008; 17:239–246.
- Matheos E, Vasileos K, Fragkiskos F, Kostas F, Kostac C. Primary omental torsion: report of two cases. Surg Today. 2009;36:64-7.