48uep6bbphidvals|364
48uep6bbph|2000F98CTab_Articles|Fulltext
Introduction
Chronic pancreatitis (CP) is a condition with continuing inflammatory disease of the pancreas, characterized by irreversible morphological change and typically causing pain and permanent loss of function. Unlike the West, idiopathic chronic pancreatitis, including tropical chronic pancreatitis (TCP), remains the predominant etiology in India, although alcoholic pancreatitis (ACP) now constitutes a significant proportion of cases (nearly a third of the cases).[1] Malnutrition has been reported in up to 50% of patients with TCP, the etiology of which is considered multifactorial. Most cases of tropical pancreatitis have been reported from Kerala state, the south-western state in India. Etiopathogenesis of tropical pancreatitis remains unclear. The initial reports of TCP by Geeverghese and colleagues suggested that malnutrition was almost an invariable feature.[2] Cassava consumption was also a hallmark in the patients of TCP reported in earlier series. The earlier prevalent view was that predominant consumption of cassava, a tuber rich in carbohydrate and poor in protein, with high cyanogens content, acted as a dietary toxin or otherwise was an index of malnutrition.[3,4] The role of cassava was discredited by a well conducted case control study.[5] A recent study indicated that malnutrition is an effect rather than a cause of TCP.[6]
Various surveys conducted by NNMB ( National Nutrition Monitoring Bureau of the National Institute of Nutrition, under Indian Council for Medical Research-ICMR) suggest that Kerala state consistently has scored high in most of the nutritional parameters in the last few decades.[7] A change in lifestyle with better availability of foodstuffs has been the general trend. Of particular note is the considerable reduction in cassava consumption by the population. A unique feature of diet in Kerala is the widespread use of coconut oil as a cooking medium which is extremely rare in other parts of India. This oil is rich in medium chain triglycerides and hence is generally regarded as beneficial in improving nutrition in CP patients.[7] A rise in alcoholism has also been reported and now Kerala state tops in per capita alcohol consumption in India.[8] These changes are perhaps reflected in a recent report on the changing phenotype of TCP observed over the past few years.[9] In this context, we sought to conduct a comprehensive anthropometric, biochemical, clinical, and dietary (ABCD) assessment of CP patients and also tried to study the association of the nutritional status of the patients with their dietary intake.
Methods
One hundred consecutive patients of CP attending the Pancreas clinic constituted the study population. CP was diagnosed by presence of typical changes in one or more maging modalities (US/CT/ERCP/EUS). Patients with CP having alcohol consumption > 80gm/day were considered to have ACP while TCP was diagnosed using previously defined criteria.[1]
All the patients were personally interviewed by a trained dietician who recorded the data. In addition all the patients were seen by the physician(s) in the clinic who ratified the recorded data.
Dietary survey
A detailed dietary history was obtained from all the patients during the interview by using a semi-quantitative food frequency questionnaire.[10] Record of all food stuff consumed during the past 24 hours was made with the recall method.[11] The results were analyzed in accordance with the standard Tables of Food Consumption in India.[12] The amounts of proteins, fats, carbohydrates, and the calories for these were computed. A comparison was made with that of NNMB data for Kerala population.[7]
Nutrient intake was calculated using the semi-quantitative food frequency questionnaire and the 24-hour recall method. Percentage of the ICMR recommended RDA of various nutrients was assessed.[13]
Nutritional assessment
Weight was measured using a beam scale with movable but non-detachable weights. The subjects were weighed without shoes when they stood erect with both hands hanging freely. The weight was recorded to the nearest 0.1gm.
Height was measured using a statiometer when the subjects were made to stand erect on the platform of weighing scales. The headpiece was held without much pressure in the sagittal plane (central part of the head) and the height measured to the nearest 0.1cm.
Body mass index was calculated dividing the weight in kg by the square of the height in m2.
Percentage weight change was computed by the formula: % weight change = [(usual weight-actual weight)/usual weight] x 100
Triceps skin fold thickness (TST) measurement: TST was measured using a standard caliper when the examiner stood behind the subject and applied the tip of the caliper to the triceps fat fold of the freely hanging non-dominant arm at a point midway between the lateral projection of the shoulder and the elbow.
Mid upper arm circumference: MUAC was measured using a tape snugly wrapped around the non-dominant arm at the midpoint.
Waist hip ratio (WHR) was measured.
Clinical signs of vitamin and micronutrient deficiency were recorded.
Modified Subjective Global Assessment: Modified SGA scores were recorded which included 7 items in medical history and 4 clinical findings.[14] Patients were classified into 3 groups: well nourished (SGA-A), moderately malnourished (SGA-B), and severely malnourished (SGA-C).
Biochemical evaluation: Serum protein, albumin, globulins, serum calcium, serum lipids, and hemoglobin were estimated. Statistical analysis was done using SPSS version 11. This study was approved by our Institutional Ethics Committee. Written informed consent was obtained from the
subjects before enrolment.
Results
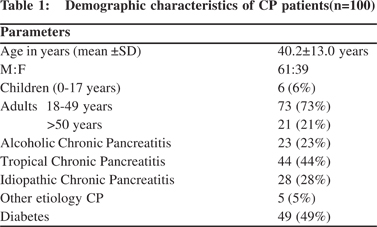
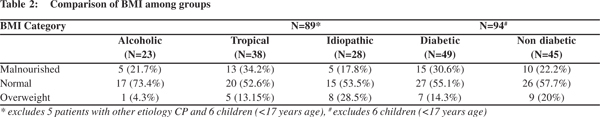
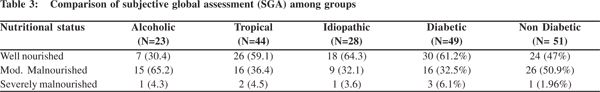
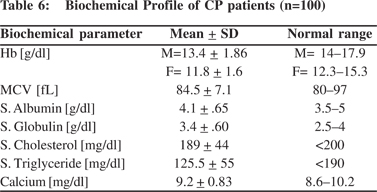
There were 44 TCP, 23 ACP, and 28 ICP patients (Table 1). 49% of the subjects were diabetic. 59% of chronic pancreatitis patients had normal BMI and 14% of patients were moderately malnourished. 27% of patients were underweight (Table 2). By subjective global assessment (Table 3), 54% of chronic pancreatitis patients were well nourished and 42% were moderately malnourished; only 4% patients were seen to have severe malnourishment. Malnutrition, detected by subjective global assessment, did not always correlate with low BMI. While MUAC (Table 4) was comparable to controls, TST (Table 5) was significantly lower in CP as compared to controls. Biochemical parameters (Table 6) were not significantly lower in CP patients.


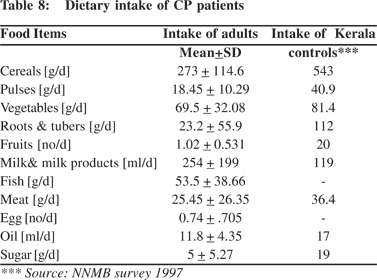
Majority of patients (96%) were non-vegetarians. However, the majority consumed non-vegetarian dishes only 1-2 times a week. The food intake of CP patients especially cereals, pulses, and fruits was low in comparison to Kerala population controls (Tables 7 and 8). Average calorie intake of males was 1389 ± 515.9 kcal and that of females were 1206 + 404 kcal (Table 7).
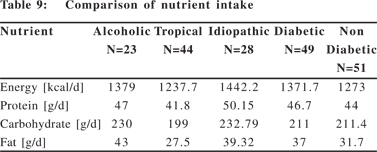
The intake of fat as well as protein was comparable in diabetics and non-diabetics (Table 8). The mean fat intake of the TCP patients was 27.5 g/day as compared to 43 g/day in ACP patients
(Table 9).
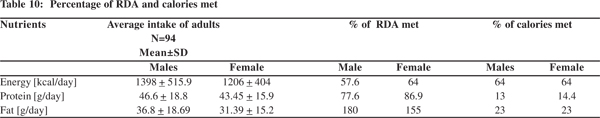
Males met 57.6 % of RDA and females met 64% of RDA (Table 10) suggesting calorie (energy) deprivation. Percentage of calories met from fat was 23% in both males and females.


Discussion
Traditionally a high fat, high protein diet has been considered harmful in alcoholic CP. Further, a low fat diet also increases the risk for CP. The Kerala diet which was predominantly a high starch, low protein, and low fat diet was an object of close scrutiny in earlier studies on TCP. Although protein malnutrition and dietary toxins like cassava are no longer regarded as dominant etiological factors, the role of other dietary factors in CP remains enigmatic. Apart from etiopathogenesis, adequate dietary assessment is integral to correction of malnutrition in CP.
In this study we undertook a comprehensive anthropometric, biochemical, clinical, and dietary (ABCD) assessment. We sought to ascertain the current prevalence of malnutrition among patients with CP in a population with a high prevalence for CP, in the context of a reported improvement in nutritional parameters in population surveys. For this reason we have tried to compare our results with those of the surveys conducted by NNMB and also tried to assess how far the nutrient intake by our patients fell below the Indian Council of Medical Research (ICMR) recommended daily allowances (RDA) for the Indian population. We have also tried to look at different parameters of malnutrition in order to ascertain the best method or best combination of methods. This is perhaps the first such study in CP patients which has tried to correlate all these parameters. Taking a holistic approach, we have sought to study the association of nutritional status with dietary intake.
We found that 23% of our patients had ACP reflecting the increase in prevalence of alcoholism. While the dietary pattern by far was predominantly a non-vegetarian diet, the actual portions of non-vegetarian dishes consumed, were modest. The food intake of CP patients was very low especially in the intake of cereals, pulses, and fruits as compared to the controls (NNMB data). It was seen that female patients met 64% of the recommended calorie requirements, while 57% of these requirements was met by males. The percentage of calories met from protein and fat were within normal ranges in both males and females. This suggests that rather than protein or fat deficiency, the main nutritional problem in our CP patients is energy (calorie) deficiency. However, fat intake in TCP patients was considerably lower as compared to ACP. We found that 51% of our CP patients were diabetic. There was no significant difference in terms of nutrient intake between diabetics and non-diabetics.
In a cohort of CP, 20 years earlier, the senior author has reported on the poor intake of fat and protein as also the increased intake of Cassava.[15] In another study by the same author, diets of TCP patients and controls from Kerala compared poorly with ACP patients and controls from France.[16]
A more recent study from northern (subtropical) India reports similar low intake of calories.[17] In this study, while 86% of CP patients were in the normal range of BMI, 67% reported weight loss after onset of disease.
We found that majority of our patients had moderate malnutrition only. In this study, the presence of severe malnutrition is only 14% based on BMI and 4% based on SGA which is much lower than the figures reported by us in a previous series where nearly 40% had severe malnutrition.[15]
On comparing the BMI, it was seen that patients with TCP were more malnourished than ACP. The BMI of diabetic and non-diabetic CP patients were comparable. However, we found that use of modified SGA identified more cases of malnutrition than BMI. We feel that SGA which is a clinical nutritional index involving a standardized questionnaire consisting of dietary intake changes, recent body weight changes, GI symptoms, functional capacity, and physical signs of malnutrition (loss of subcutaneous fat or muscle mass, edema, ascites), is the single most useful tool in assessment of malnutrition in CP. Wakahara et al have previously shown that nutritional screening with SGA predicts hospital stay in patients with digestive diseases.[18] Recently Filipoviæ et al have also reported a higher ensitivity for SGA.[19]
The use of anthropometric measurements like triceps skin fold measurement, waist hip ratio, mid arm circumference especially TST are useful when used in conjunction with BMI to detect malnutrition. Clinical signs suggesting deficiency of vitamins and micronutrients were seen in this population. However, florid signs indicating severe deficiency were seen only in a minority. Biochemical parameters like serum albumin and hemoglobin do not appear to be particularly helpful in assessment of malnutrition in CP.
A recent RCT suggests that dietary counseling for a balanced home diet is as good as MCT enriched commercial food supplements.[20] While dietary counseling by a trained dietician would be ideal, it may not be feasible in many centers providing primary care to CP patients. Malnutrition in CP is multifactorial - the low protein, high carbohydrate content of the diet, steatorrhea, poor intake of food due to fear of pain, uncontrolled diabetes mellitus, and micronutrient deficiency contributing to varying degrees. The main concern in nutritional rehabilitation lies in making a distinction between patients in whom steatorrhea and consequent maldigestion is the chief cause of malnutrition as compared to other causes. We have recently reported abnormalities in zinc status in CP which correlated with exocrine and endocrine insufficiency.[21]
We have also reported for the first time that homocysteine was seen to be a risk factor in CP patients and was consequent to folate deficiency.[22] In a recent study on estimation of fecal elastase-1 and acid steatocrit in chronic pancreatitis, we found that fecal elastase-1 correlated with fecal fat excretion and BMI. Furthermore evidence of pancreatic insufficiency was found in about half of the patients with normal BMI in the same study.[23]
While dietary counseling remains a cornerstone in the treatment of malnutrition in CP, the need for selective supplementation of micronutrients like zinc, folate, etc. needs closer scrutiny. Optimization of pancreatic enzyme replacement therapy may be more feasible by incorporation of objective measures of pancreatic insufficiency like fecal elastase-1 and acid steatocrit. The role of dietary factors especially in tropical pancreatitis cannot be totally negated.
References
1. Balakrishnan V, Unnikrishnan AG, Thomas V, Choudhuri G, Veeraraju P, Singh SP, et al. Chronic pancreatitis. A prospective nationwide study of 1,086 subjects from India. JOP. 2008;9:593–600.
2. Geeverghese PJ. Calcific pancreatitis: causes and mechanisms in the tropics compared with those in the subtropics. Trivandrum: St. Joseph’s Press,1986.
3. McMillan DE, Geevarghese PJ. Dietary cyanide and tropical malnutrition diabetes. Diabetes Care. 1979;2:202–8.
4. Sandhyamani S. Role of dietary factors in the etiology of fibrocalculous pancreatic disease and diabetes. In: Balakrishnan V editor. Chronic pancreatitis and pancreatic diabetes in India. Kochi: Indian Pancreatitis Study Group; 2006. P. 294-313. Available from:http://www.ipans.org/ Publications/chapter22.pdf
5. Narendranathan M, Cheriyan A. Lack of association between cassava consumption and tropical pancreatitis syndrome. J Gastroenterol Hepatol. 1994;9:282–5.
6. Midha S, Singh N, Sachdev V, Tandon RK, Joshi YK, Garg PK. Cause and effect relationship of malnutrition with idiopathic chronic pancreatitis: prospective case-control study. J Gastroenterol Hepatol. 2008;23:1378–83.
7. National Nutrition Monitoring Bureau (NNMB) survey 1997.
8. Das SK, Balakrishnan V, Vasudevan DM. Alcohol: its health and social impact in India. Natl Med J India. 2006;19:94–9.
9. Balakrishnan V, Nair P, Radhakrishnan L, Narayanan VA. Tropical pancreatitis - a distinct entity, or merely a type of chronic pancreatitis? Indian J Gastroenterol. 2006;25:74–81.
10. Beal VA. The nutritional history in longitudinal research. J Am Diet Assoc. 1967;51:426–32.
11. Burke BS. The dietary history as a tool in research. J Am Diet Assoc.1947;23:1041–7.
12. Gopalan C, Ramasastri CV, Balasubramanian SC. Nutritive value of Indian foods. Revised and updated by Narasinga Rao BS, Deosthale TG, and Pant KC. Indian Council of Medical Research. 1993.
13. Nutrient requirements and recommended daily allowance for Indians. Indian Council of Medical Research. 1990;129.
14. Baker JP, Detsky AS, Wesson DE, Wolman SL, Stewart S, Whitewell J, et al. Nutritional assessment: a comparison of clinical judgment and objective measurements. N Engl J ed. 1982;306:969–72.
15. Balakrishnan V, Hariharan M, Sindhu S. Pathogenesis of pancreatitis in India leading on to diabetes mellitus. Proc Nutr Soc India. 1990;36:1–7.
16. Balakrishnan V, Sauniere JF, Hariharan M, Sarles H. Diet, pancreatic function, and chronic pancreatitis in South India and France. Pancreas. 1988;3:30–5.
17. Singh N, Joshi YK, Saraya A, Tandon RK. Nutritional profile of patients with chronic pancreatitis. Asia Pacific J Clin Nutr. 1999;8:19–23.
18. Wakahara T, Shiraki M, Murase K, Fukushima H, Matsuura K, Fukao A, et al. Nutritional screening with Subjective Global Assessment predicts hospital stay in patients with digestive diseases. Nutrition. 2007;23:634–9.
19. Filipoviæ BF, Gajiæ M, Miliniæ N, Milovaniæ B, Filipoviæ BR, Cvetokoviæ M, et al. Comparison of two nutritional assessment methods in gastroenterology patients. World J Gastroenterol. 2010;16:1999–2004.
20. Singh S, Midha S, Singh N, Joshi YK, Garg PK. Dietary counseling versus dietary supplements for malnutrition in chronic pancreatitis: a randomized controlled trial. Clin Gastroenterol Hepatol. 2008;6:353–9.
21. Girish BN, Rajesh G, Vaidyanathan K, Balakrishnan V. Zinc status in chronic pancreatitis and its relation with exocrine and endocrine insufficiency. JOP. 2009;10:651–6.
22. Girish BN, Vaidyanathan K, Rao NA, Rajesh G, Reshmi S, Balakrishnan V. Chronic pancreatitis is associated with hyperhomocysteinemia and derangements in transsulfuration and transmethylation pathways. Pancreas. 2010;10:e11–6.
23. Girish BN, Rajesh G, Vaidyanathan K, Balakrishnan V. Fecal elastase1 and acid steatrocrit estimation in chronic pancreatitis. Indian J of Gastroenterol. 2009;28:201–5.