48uep6bbphidvals|352
48uep6bbph|2000F98CTab_Articles|Fulltext
Malaria still continues to be a major health problem in many parts of the world. An enlarged spleen is considered to be one of the cardinal physical signs. Though splenic rupture in malaria is rare but yet it is a important life threatening complication specially of Plasmodium vivax. Spontaneous splenic rupture has been described in conditions such as infectious mononucleosis, haematological malignancies[1,2,3] but malaria continues to be the most common aetiology.[4,5]
Traditionally all types of splenic rupture have been treated with splenectomy but with the emerging trend of splenic conservation in splenic trauma similar approach has been applied to a ruptured malarial spleen also. We report a patient with combined P.falciparum and P.vivax malaria who developed spontaneous splenic rupture and was managed successfully non–operatively.
Case Report
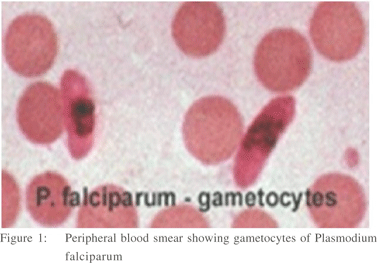
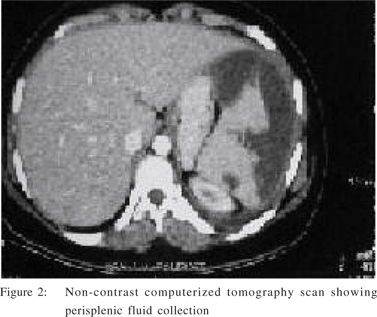
A seventeen year old girl presented to the emergency department with history of intermittent high grade fever for the last eight days. The fever was associated with chills and rigors. This was followed by abdominal pain, distension and repeated episodes of non bilious vomiting for the last 3 days. At presentation she had a pulse of 102 per minute, respiratory rate of 24 per minute, and mild hypotension (98/60 mm) .On examination, abdomen was distended with tenderness in left hypochondrium. Spleen was palpable 3 cm below the left costal margin and liver was palpable 4 cm below the right costal margin. There was evidence of free fluid in the abdomen and the bowel sounds were sluggish. On investigations her haemoglobin was 7.2 g% with thrombocytopenia (platelet count of 42,000 per cu mm) and marked leukocytosis (total leukocyte count of 25,000 per cu mm). The blood urea was 184 mg/dl and serum creatinine was elevated {5.7 mg% (normal 0.8-1 mg %)}. A peripheral blood smear showed gametocyte of Plasmodium falciparum(Figure 1). An antibody enzyme linked immunosorbent assay (ELISA) was positive for both P.falciparum and P.vivax. Ultrasonography and non contrast computerised tomography scan (Figure 2) revealed a wedge shaped infarct in the spleen with free fluid in the abdomen suggestive of splenic rupture. The patient was put on conservative management with monitoring of vitals, laboratory parameters and clinical signs. An infraumblical abdominal drain was inserted which drained about 600 ml of non clotting blood. Patient was started on injection artesunate 120 mg and broad spectrum antibiotic (imepenem 1 gram and cilastatin 500 milligrams). She was transfused blood and blood products and underwent one haemodialysis. Subsequently she went into diuretic phase of renal failure and her renal parameters improved within next two weeks. Her general condition gradually started improving. Peripheral blood smear showed a decrease in gametocyte counts (200/cu mm). The anti malarials and antibiotics were stopped after 2 weeks and patient made an uneventful recovery .She is on regular follow up and a contrast enhanced CT scan done after 4 weeks showed a collection around the spleen . A repeat ultrasound after three months showed complete resolution and no collection and patient is asymptomatic after 9 months of follow up.
Discussion
Spleen plays an important role in the host defence against number of intravascular parasites including Plasmodium. Traumatic splenic rupture is a well described entity but spontaneous splenic rupture has also been described. It has been describeed in few diseases such as infectious mononucleosis, splenic neoplasm and haematological malignancies.[1,2,3] However, malaria is by far the most common cause of spontaneous splenic rupture. Splenic involvement in malaria causes splenomegaly which makes it more prone to rupture.[6,7] Other splenic complications of malaria that have been described include the hyperactive malarial spleen (tropical splenomegaly syndrome), hypersplenism, splenic cysts and splenic torsion.
The incidence of spontaneous rupture of spleen in malaria has been estimated to be about 2%[8,9,10] and it has been reported that the incidence is higher in induced malaria (via blood transfusions) as compared to natural malaria (mosquito bite/ transplacental). A total of 22 cases have been reported since 1960[5,6,13,14,15,16,17,18,19]. This spontaneous rupture almost exclusively occurs during the stage of acute infection and most commonly during the primary attack[11,12] as seen in our case. The malarial species most commonly involved is P.vivax though rare cases of P falciparum and malaria have also been reported.[11] However no case of spontaneous rupture has been described in combined P.falciparum and P.vivax malaria as in our case.
The exact mechanism of spleen rupture in malaria is not known. The following three mechanisms are implicated:(i) increase in intrasplenic tension due to cellular hyperplasia and engorgement; (ii) spleen may be compressed by the abdominal musculature during physiological activities such as sneezing, coughing, defecation, etc.; and (iii) vascular occlusion due to reticulo-endothelial hyperplasia, resulting in thrombosis and infarction. This leads to interstitial and subcapsular haemorrhage and stripping of the capsule, which lead to further subcapsular haemorrhage. The distended capsule finally gives way.[11]
The common presenting features are fever, tachycardia, vomiting, generalized abdominal pain, progressive weakness. However splenic rupture in malaria continues to be a real pitfall for practitioners for it can happen without any preceding attacks or trauma. Physical examination may reveal tenderness in left hypochondrium, enlarged spleen and signs of diaphragmatic irritation (Kehr’s sign). Signs of hypotension and hypovolemic shock may also be present. The tests usually carried out for diagnosis of splenic rupture include abdominal sonography, Contrast Enhanced CT scan of abdomen which will reveal enlarged spleen, capsular tear and perisplenic hematoma.
Historically the treatment of splenic rupture has been splenectomy7. With the emergence of splenic conservation in splenic trauma similar concept has been applied to spontaneous rupture in other conditions. As our patient was young, haemodynamically stable and considering the immunological role of spleen in pneumococcal and malarial infection , we opted for a non-operative management. The conservative management consists of observation for 7-14 days in hospital with strict bed rest, administration of blood and blood products,[6,7] serial monitoring of haemoglobin and haematocrit along with monitoring of vital parameters. Regular abdominal ultrasonography should be done to assess the progress of the patient. Splenectomy should be reserved for patients with uncontrolled bleeding and haemodynamic instability.
In conclusion, spontaneous splenic rupture of malarial spleen is rare and requires high degree of clinical suspicion to arrive at a diagnosis. Most of these cases, like traumatic splenic injuries, can now be managed non-operatively. Splenic salvage should be the aim in the management of these patients.
References
1. Baralkiewicz G, Mijal J, Karan J, Rybski Z, Juszczyk J. Spontaneous splenic rupture as a complication of infections mononucleosis. Przegl Epidemiol. 1996;50:435–41.
2. Alberty R. Surgical implications of infectious mononucleosis. Am J Surg. 1981;141:559–61.
3. Pettersen JT, Modalsli O, Solheim K, Buanes T. Splenic neoplasms. Tidsskr Nor Laegeforen. 1993;113:1468–9.
4. Yagmur Y, Kara IH, Aldemir M, Buyukbayram H, Tacyildiz IH, Keles C. Spontaneous rupture of malarial spleen: two case reports and review of literature. Crit Care. 2000;4:309–13.
5. Bucinto R, Kald A, Borch K. Spontaneous rupture of spleen. Eur J Surg. 1992;158:129–30.
6. Clezy JK, Richens JE. Non-operative management of a spontaneously ruptured malarial spleen. Br J Surg. 1985;72:990.
7. Mokashi AJ, Shirahatti RG, Prabhu SK, Vagholkar KR. Pathological Rupture of malarial spleen. J Postgrad Med. 1992;38:141–2.
8. Martelo OJ, Smoller M, Saladin TA. Malaria in American soldiers. Arch Intern Med. 1969;123:383–7.
9. Khan MY, Zinneman HH, Hall WH. Vietnam malaria: Clinical experience with 50 patients. Minn Med. 1970;53:331–4.
10. Howard WA, Krotoski WA, Slonim MS, Contacos PG. Spontaneous splenic rupture in vivax malaria: case report. Mil Med. 1973;138:32–5.
11. Zingman BS, Viner BL. Splenic complication in malaria: case report and review. Clin Infect Dis. 1993;16:223–32.
12. Baidas WH, Al-Zamil A, Mathew CV. Spontaneous rupture of a malarial spleen. Annals Saudi Med. 1999;19:139–40.
13. Bearn JG. Spontaneous rupture of malarial spleen. A case report and some anatomical and pathological considerations. Trans R Soc Trop Med Hyg. 1961;55:242–5.
14. Martelo OJ, Smoller M, Saladin TA. Malaria in American soldiers. Arch Intern Med. 1969;123:383–7.
15. Davis R. Spontaneous rupture of the pathological spleen in malaria. S Afr Med J. 1973;47:1801–3.
16. Walzer PD, Gibson JJ, Schwltz MG. Malaria fatalities in the United States. Am J Trop Med Hyg. 1974;23:328–33.
17. Touze JE, Garnotel E, Martet G, Ducourau JP, Beauté D, Zimmermann JC, et al. Spontaneous spleen rupture in malaria. Trans R Soc Trop Med Hyg. 1989;83:161.
18. Falk S, Protz H, Kobrich U, Stutte HJ. Spontaneous splenic rupture in acute malaria tropica. Dtsch Med Wochenschr. 1992;117:854–7.
19. Tauro LF, Maroli R, D’Souza CR, Hegde BR, Shetty SR, Shenoy D. Spontaneous rupture of the malarial spleen. Saudi J Gastroenterol. 2007;13:163–7.