Tony Jose1, Biju I K1, Anish Kumar1, Sajeesh Sahadevan2, Ramesh Bhasi3, Ramakrishnan KG4, Lilly M5, Shalini Kuruvila5, Abdulla Cherayakkatt6
1Department of Gastroenterology
2Department of Surgical Gastroenterology
3Department of Rheumatology
4Department of Radiodiagnosis
5Department of Pathology
6Department of General Medicine
MIMS Hospital,
Govindapuram, Calicut, India.
Corresponding Author:
Dr. Tony Jose
Email: doctonyjose@yahoo.co.in
DOI:
http://dx.doi.org/
48uep6bbphidvals|277 48uep6bbphidcol4|ID 48uep6bbph|2000F98CTab_Articles|Fulltext Polyarteritis nodosa (PAN) is a form of vasculitis that affects several organs including the gastrointestinal tract and liver.[1] Microaneurysms seen on arteriography are characteristic and tissue biopsy is confirmatory for PAN. Gastrointestinal and liver involvement occurs in 14% to 65% of patients with PAN.[2] Postprandial abdominal pain resulting from ischemia is the most common manifestation.[2] Rarely, instances of bowelperforation,[3] bleeding,[4] and acalculous cholecystitis[5] may also develop.
Case Report
A 43-year-old man was admitted with sudden onset of abdominal pain. There was no significant history of past illness. On clinical evaluation, the patient was in agony and had tachycardia, tachypnoea and hypotension. Abdominal examination revealed generalised rigidity and tenderness. Routine investigations demonstrated hemoglobin of 12.6 g%, total leukocyte count of 11,500 cells/mm3, and ESR 98 mm/ hour. Plain x-ray abdomen revealed gas under the diaphragm and an emergency CT scan showed pneumoperitoneum. The patient was resuscitated with fluids, inotropic and ventilatory support. Renal and liver function tests were normal. Emergency laparotomy was conducted which showed a perforation in the sigmoid region with massive contamination of the peritoneum with fecal matter. The patient was treated with peritoneal lavage, bowel loop exteriorisation and a tube drain. In addition, a biopsy was taken from the site of perforation.
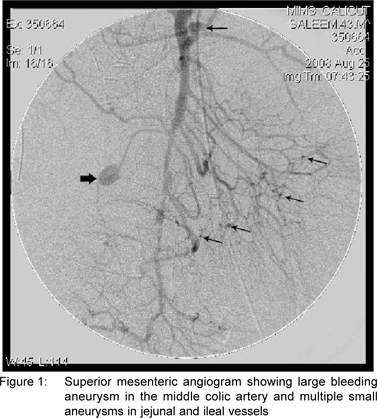
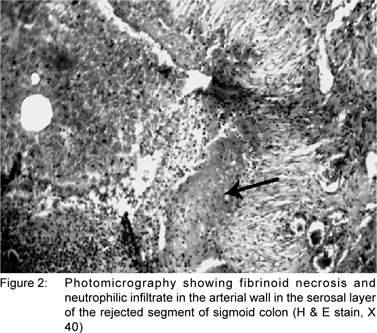
A few hours later, the patient developed massive bleeding through the drain. A repeat CT scan done showed a collection in the transverse mesocolon. Re-exploration was done and a large hematoma evacuated from the mesocolon. But after two days, the patient again developed bleeding through the drain. An arteriogram was performed and a bleeding aneurysm in the middle colic artery and multiple small aneurysms in the intestinal vasculature were seen (Figure 1). At the third exploration the middle colic artery was ligated and the bleeding was controlled. The patient had a stormy postoperative period due to sepsis. But he improved with ventilatory support, broad spectrum antibiotics and other supportive measures. Biopsy from the site of perforation was consistent with arteritis (Figure 2). p-ANCA was positive. He was started on prednisolone 50 mg/d orally and improved well within two weeks. Azathioprine 50 mg/d orally was added later and prednisolone was tapered slowly. He has been asymptomatic for the last six months.
Discussion
PAN is a focal segmental necrotising vasculitis affecting smalland medium-sized vessels. It predominantly affects middleaged men. Fibrinoid necrosis of vessels leads to microaneurysm formation mainly in renal, cerebral and coronary vessels. This can manifest as infarction, haemorrhage and progressive organ failure.[6] PAN can be primary or secondary to viral infections like hepatitis B.[7] Histology showing focal fibrinoid necrotising vasculitis involving small- and medium-sized vessels is confirmatory of PAN. Arteriogram or computed tomography angiography demonstrating microaneurysms involving renal and intestinal vasculature and positive p-ANCA are other characteristic features.[8] Treatment is with steroids and immunosuppressants like cyclophosphamide.[9] Infection associated PAN is treated best with antiviral agents.
Gastrointestinal and hepatobiliary involvement is not uncommon in PAN. Our patient initially presented with sigmoid perforation and he developed bleeding from the middle colic artery during hospital stay. Abdominal pain resulting from progressive ischemia is the main symptom in PAN patients. There are case report of colorectal ulcerations in these patients.[10] Gambino et al[1] reported isolated involvement of the large intestine in a patient with polyarteritis nodosa. There are case reports of PAN patients with acalculous cholecystitis,[5] acute pancreatitis with pseudocyst formation,[11] acute appendicitis,[12] and necrotising vasculitis of mesentery.[13] There are two case reports of haemorrhage due to rupture of the middle colic artery in polyarteritis nodosa patients.[14,15]Biliary stricture[16] and massive upper gastrointestinal haemorrhage[17] are some other rare manifestations. There are some reports of intestinal perforation in these patients.[18,19] Okada et al reported sigmoid colon perforation in polyarteritis nodosa.[20] To the best of our knowledge, this is the first report of a patient with sigmoid colon perforation and middle colic artery aneurysm rupture.
References
1. Gambino G, Rizzuto MR, Spallitta IS, Rizzo A, Branca M, Guccione M et al. Isolated polyarteritis nodosa of the large bowel: a case report. Chir Ital. 2008;60:469–73.
2. Ebert EC, Hagspiel KD, Nagar M, Schlesinger N. Gastrointestinal involvement in polyarteritis nodosa. Clin Gastroenterol Hepatol. 2008;6:960–6.
3. Chattopadhyay A. Intestinal perforation due to polyarteritis nodosa. Indian J Pediatr. 2001;68:297–8.
4. Cooper SC, Olliff SP, McCafferty I, Wigmore SJ, Mirza DF. Polyarteritis nodosa, presenting as life-threatening gastrointestinal hemorrhage in a liver transplant recipient. Liver Transpl. 2008;14:151–4.
5. Gorgun E, Ozmen V. Acalculous gangrenous cholecystitis in a young adult: a gastrointestinal manifestation of polyarteritis nodosa. Surg Laparosc Endosc Percutan Tech. 2002;12:359–61.
6. Guillevin L, Lhote F. Polyarteritis nodosa and microscopic polyangiitis. Clin Exp Immunol. 1995;101 Suppl 1:22–3.
7. Baig S, Alamgir M. The extrahepatic manifestations of hepatitis B virus. J Coll Physicians Surg Pak. 2008;18:451–7.
8. Das CJ, Pangtey GS. Images in clinical medicine. Arterial microaneurysms in polyarteritis nodosa. N Engl J Med. 2006;355:2574.
9. Guillevin L, Pagnoux C. Treatment of systemic vasculitides. Rev Prat. 2008;58:541–4.
10. Sano F, Miyamae T, Nakagishi Y, Kinoshita J, Ozawa R, Imagawa T, et al. Gastrointestinal involvement and renal infarction in a boy with classic polyarteritis nodosa diagnosed with 3D-computed tomography angiography. Nihon Rinsho Meneki Gakkai Kaishi. 2008;31:415–21.
11. Suresh E, Beadles W, Welsby P, Luqmani R. Acute pancreatitis with pseudocyst formation in a patient with polyarteritis nodosa. J Rheumatol. 2005;32:386–8.
12. Misdraji J, Graeme-Cook FM. Miscellaneous conditions of the appendix. Semin Diagn Pathol. 2004;21:151–63.
13. Dewar CL, Bellamy N. Necrotizing mesenteric vasculitis after long standing cutaneous polyarteritis nodosa. J Rheumatol. 1992;19:1308–11.
14. Dutton-Gaddis JG, Oyekan TB, Haraway GD, Crapse FJ. Middle colic artery rupture in a patient with ANCA associated vasculitis: a case report. J Okla State Med Assoc. 2004;97:364–6.
15. Hixson R, Calder F, Watson D. Middle colic artery rupture: an unusual presentation of polyarteritis nodosa. Br J Rheumatol. 1997;36:819–20.
16. Barquist ES, Goldstein N, Zinner MJ. Polyarteritis nodosa presenting as a biliary stricture. Surgery. 1991;109:16–9.
17. Perez RA, Silver D, Banerjee B. Polyarteritis nodosa presenting as massive upper gastrointestinal hemorrhage. Surg Endosc. 2000;14:87.
18. Siegenthaler H, Egger G. Perforation of the small intestine during a course of nodose polyarteritis: an unusual complication. Schweiz Rundsch Med Prax. 1972;61:836–40.
19. Roikjaer O. Perforation and necrosis of the colon complicating polyarteritis nodosa. Case report. Acta Chir Scand. 1987;153:385–6.
20. Okada M, Konishi F, Sakuma K, Kanazawa K, Koiwai H, Kaizaki Y. Perforation of the sigmoid colon with ischemic change due to polyarteritis nodosa. J Gastroenterol. 1999;34:400–4.
|