48uep6bbphidvals|202
48uep6bbphidcol2|ID
48uep6bbph|2000F98CTab_Articles|Fulltext
In spite of tremendous advances in medical management there remains a subset of peptic ulcer patients who present with gastric outlet obstruction requiring surgical intervention. In this situation truncal vagotomy and drainage either by the open method or by laparoscopy remains a therapeutic option with good long term results and a low incidence of complications.1 A 5-10% recurrence rate is mostly attributable to incomplete vagotomy.[1] When such patients return with symptoms it is necessary to assess if the previous vagotomy was complete.
Studies in the past have reported abolition of the postprandial alkaline tide as a simple, easy to perform and reliable test for estimating how complete the vagotomy was.[2,3] However, other reports have dismissed urinary compensation for gastric acid secretion as being too small to be of any physiological or clinical significance.[4] In addition, a consistent lack of this response to H2-receptor antagonists or proton pump inhibitor-mediated gastric acid suppression has led scholars to question the basis of the postprandial alkaline tide.[5] There is also controversy concerning the influence of the nature of the test meal on the postprandial urinary response.
This study was carried out to answer the following questions: a) Is the postprandial urinary alkaline tide dependent on the nature of the test meal, i.e. solid or liquid? b) What is the effect of proton pump inhibitor therapy on postprandial alkaline tide? c) Can abolition of postprandial alkaline tide be used as a reliable bedside test for assessing the completeness of vagotomy?
Methods
The study was conducted at the Department of Surgery, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry, over a period of 2 years. The postprandial urinary alkaline tide (PUAT) pattern was prospectively assessed in three different study groups and one control group of healthy volunteers. The three study groups were as follows:
· Group A (n=20) Proton Pump Inhibitor (PPI) Group: Consecutive patients with endoscopically confirmed ctive symptomatic non-obstructed duodenal ulcer who underwent PUAT before and after a ten-day course of PPI (omeprazole, 20 mg BD).
· Group B (n=25) Truncal Vagotomy (TV) Group: Consecutive patients with endoscopically proven duodenal ulcer and gastric outlet obstruction who underwent PUAT before and after truncal vagotomy and drainage.
· Group C (n=5) Recurrent Ulcer (RU) Group: Patients with endoscopically proven recurrent duodenal or stomal ulcer after a previous truncal vagotomy and drainage.
Patients with combined duodenal ulcer and gastric ulcerwere excluded.
For the preoperative test in patients with gastric outlet obstruction who could not retain a solid diet (15 out of 25) a standard liquid diet was used. For the remaining ten a standardsolid diet was used. In the present study we used a standard test meal prepared in our Institute kitchen. It consisted of 150 g of rice, 20 g sambar and 2 boiled eggs. The cost of the diet was approximately Rs.12 per meal. The diets used by Ahmad[2] and Johnson5 consisted of meat and fish which had a much higher protein content as compared to our diet. However the cost of their diet was also higher.
Since many of the patients in Group C with gastric outlet obstruction could not tolerate the solid standard diet we tried to standardise a liquid diet for these patients. It consisted of 200 mL cow’s milk, 200 mL sago water and 200 mL of ragi gruel.
Three days before the test all medications were withdrawn. On the night before the test, patients were allowed a standard diet and nothing by mouth thereafter. Patients were instructed to empty their bladder the next morning and subsequently a 20 mL urine sample was collected for measuring the fasting urinary pH. Patients then received a standard test meal and postprandial urinary pH was measured in a sample collected after two hours.
In the past, many workers had used urinary acid output to measure the alkaline tide.[5] We studied the urine acid output in a few healthy volunteers in our Institute.[6] We found that the urine acid output was influenced by the subject’s general condition and the diet he or she consumed. It was also found that the urine acid output varied from day to day and was difficult to standardise. Hence, urine pH was selected instead of urinary acid output as the test parameter in our study.
Urinary pH was measured by a pocket digital pH meter (HANNA Company, Germany, pH range 0-14 with resolution of 0.1).
Data was analysed using Student’s paired ‘t’ test, Wilcoxon matched paired signed rank test and Mann Whitney U test (Instat 3). Results are presented as mean ± standard deviation. A p value of less than 0.05 was taken as significant.
The study was approved by the Institute Research Council and Ethics Committee.
Results
A total of 50 patients in three study groups and 20 controls were studied. The control group was matched for age and gender.
Fasting urinary pH was higher in all study groups when compared with controls and this difference was significant in all except Group C, probably because there were only five patients in this group. (Table 1)
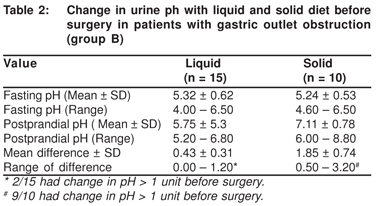
On comparing the effect of the nature of the test meal (solid vs. liquid) on the urine pH before surgery in the gastric outlet obstruction group, it was seen that with a solid test meal, 9 out of 10 patients showed a positive preoperative alkaline tide in contrast to the finding seen with a liquid diet where only 2 out of 15 patients demonstrated a change in pH. This indicated that liquid diet may not be effective at all in evaluating an alkaline tide prior to surgery. (Table 2)
Measurement of the postprandial urinary alkaline tide in the control group showed a significant increase in the urinary pH when compared to the fasting state. The mean increase was 1.59 ± 0.47 units and none of the patients demonstrated a change of less than 1 unit. This may be taken as a cut-off point for positivity of postprandial alkaline tide in normal controls with intact vagi. (Table 3)
On studying the effect of proton pump inhibitors on acid secretion it was found that there was a statistically significant fall in both fasting urinary pH (5.34 ± 0.70 vs. 4.80 ± 0.61, p = 0.031) and postprandial alkaline tide (6.99 ± 0.79 vs 4.94 ± 0.63, p = 0.0001). This showed that PPIs abolish the alkaline tide and therefore must be discontinued before its measurement. Three subjects had a change in urinary pH less of than 1 unit. Table 3 also shows that after 10 days of PPI therapy none of the patients showed an alkaline tide after a meal.
When the change in the urinary pH before and after truncal vagotomy and gastrojejunostomy was studied in the group with chronic duodenal ulcer and gastric outlet obstruction it was found that there was a significant fall in the mean fasting urinary pH following surgery (5.28 ± 0.58, vs. 4.92 ± 0.66, p = 0.032). It was also seen that there was a significant decrease in the postprandial pH following surgery (6.29 ± 0.92 vs. 5.09 ± 0.73, p = 0.0001)
However, in 14 out of 25 patients the expected alkaline tide before surgery did not occur. This was attributed to the fact that these patients were unable to ingest a standard test meal due to gastric outlet obstruction. After surgery, two patients continued to show alkaline tide. Biopsy report of the excised vagi in them did not show nerve fibres, indicating that incomplete vagotomy was the cause of the persistent alkaline tide.
On comparing the change in urinary pH in patients with recurrent ulcer it was found that the mean fasting pH was 5.4
± 0.73. It changed to 5.52 ± 0.83 after a standard meal. The change in pH was 0.12 ± 0.21, which was not statistically
significant. None of the patients showed an alkaline tide, thus indicating that incomplete vagotomy was probably not the cause of recurrent ulcer. (Table 3)
Discussion
The prevalence of acid peptic disease has fallen over the last two decades in the western world, but a similar rate of decline has not yet been seen in the Asian subcontinent.[7] Truncal vagotomy with gastrojejunostomy remains one of the procedures offered to patients with chronic duodenal ulcer with gastric outlet obstruction constituting about 3 to 5% of the total elective laparotomies in our hospital. One of the problems with truncal vagotomy and gastrojejunostomy is a reported incidence of 5 to 10% ulcer recurrence after surgery.[1] The majority of these ulcers are due to incomplete vagotomy.[1,2]
There are many tests to assess the completeness of vagotomy both intraoperatively and postoperatively. Yet due to their practical limitations and theoretical drawbacks, they have not been widely accepted.[8,9] Postprandial alkaline tide is the observed alkalinity of the urine following a test meal. It is a normal physiological occurrence which has been explained by the HCO3 ion formed by the dissociation of H2CO3 to H+ + HCO3.[7] The HCO3 released into the circulation is in proportion to the acid formed and therefore must logically diminish following vagotomy.[10] Measurement of urinary postprandial alkaline tide is a simple and easy test to perform and it does not have the drawbacks of conventional tests such as the Hollander’s or the Sham Feeding Test.
In our study, the mean difference in urinary pH between the fasting and postprandial urine samples was 1.59 ± 0.47 which is much lower than the change observed by some others.[2,11] However, our findings were similar to those of Dubey,[6] who found a mean difference in pH of 1.9 units. The difference in the magnitude of change in urinary pH between the present study and that of Ahmad[2] and Johnson[4] might have been due to the higher content of protein in the diet used in their studies. We chose this diet because it was similar to the normal South Indian diet which was more acceptable to our patients and hence was more likely to show the normal physiological response in our population.
In our study, the fasting urinary pH of the controls was 4.69 ± 0.46. The fasting urinary pH was significantly higher inpatients with acute and chronic duodenal ulcers at 5.34 ± 0.7 and 5.28 ± 0.58, respectively, when compared with the controls. There was no significant difference in fasting urinary pH between controls and patients with recurrent ulcer. The reason for the higher urinary pH in patients with duodenal ulcer could be due to a higher level of basal acid output. The increase in resting pH was abolished in patients with recurrent ulcer following truncal vagotomy and drainage. Ahmad found a fasting urinary pH of 4.7 ± 0.2 in healthy volunteers as compared to 4.9 ± 0.4 in patients with chronic duodenal ulcer.[2] Dandapat et al[12] also reported similar findings. In both studies, the fasting urinary pH was higher in patients with duodenal ulcer than in healthy controls. Both studies, however, did not compare the fasting urinary pH in different groups.
In patients with active duodenal ulcer the mean postprandial rise in pH was 1.65 ± 0.89 units over the fasting value. Three of the patients had a change in urinary pH of less than 1. This may be because these patients might have had a persistently high level of the PPI in their blood, owing to the delayed metabolism of the drug in their body.[13] This postprandial rise in urinary pH as observed by other workers was 2.9 units by Ahmad et al,[2] 3.1 units by Dandapat[12] and 2.11 units by Dubey.[6]
Following a course of PPIs for ten days in patients with active duodenal ulcer without obstruction, the mean difference between the fasting and the postprandial urinary pH decreased to 0.14 ± 0.45 from 1.65 ± 0.89 (p = 0.0001). Thomas et al[14] found a direct correlation between gastric acid secretion and postprandial alkaline tide which was abolished after a course of ranitidine.
In this study, 14 out of 25 patients with chronic duodenal ulcer and gastric outlet obstruction had a change in postprandial urinary pH of less than 1 over the fasting value before surgery. The cause of this may be intolerance to the standard test meal in patients with gastric outlet obstruction. Overall, the mean change in urinary pH between fasting and postprandial value was 1.0 ± 0.88 before surgery.
Amongst the patients with chronic duodenal ulcer and gastric outlet obstruction who could tolerate solid diet, the postprandial alkaline tide was measured using a solid meal. Nine out of the 10 patients had a change in urinary pH of more than 1 indicating that solid diet was effective in eliciting postprandial alkaline tide in patients with chronic duodenal ulcer and gastric outlet obstruction, provided the patients could tolerate the diet.
After surgery, the mean difference between the fasting and postprandial urinary pH was 0.16 ± 0.33. Two patients had a positive postprandial alkaline tide postoperatively. Their postoperative biopsy report of excised vagi did not show nerve fibres. Ahmad found a mean rise in postprandial pH of 0.7 units in 89 of the 95 duodenal ulcer patients following truncal vagotomy.[2] Six of his patients had a rise in postprandial urinary pH of more than 1 unit. Hollander’s test was also positive in these six patients. Biopsy report showed incomplete vagotomy in all the six cases. Dubey[6] reported similar findings. In the present study, we did not do Hollander’s test in those patients with positive postoperative postprandial alkaline tide in the completeness of vagotomy was confirmed by the postoperative biopsy report. Secondly, the reported complications of the Hollander’s test has precluded its routine use.
Ahmad in his study found that all 3 patients who had a radiologically proven recurrent ulcer after truncal vagotomy and drainage procedure had a positive alkaline tide with a mean difference of 3 units between the fasting and the postprandial urinary pH.[2] Hollander’s test was also positive in all the three patients. During re-laparotomy, he found intact vagi in all the three cases. He concluded from his study that incomplete vagotomy was the most common cause of recurrent ulcer. However, in our study the findings were contrary to the previous study. We carried out postprandial alkaline tide test in 5 patients with endoscopically proven recurrent ulcer after truncal vagotomy and gastrojejunostomy. All five patients showed negative alkaline tide with a mean change in urinary pH of 0.12 ± 0.21 units between fasting and the postprandial value indicating that incomplete vagotomy was not the cause of recurrent ulcer after truncal vagotomy and gastrojejunostomy.
Conclusion
1. The nature of the test meal affects the postprandial urinary pH response and hence this test is not valuable for preoperative assessment in patients with gastric outlet obstruction.
2. A liquid meal is not effective in stimulating an alkaline tide.
3. The postprandial alkaline tide is abolished by proton pump inhibitors. Hence these must be discontinued at least three days before the test.
4. PUAT is a useful test for assessing the post vagotomised stomach. Most patients with a positive postprandial response will have had an incomplete vagotomy.
References
1. Srinivasan K, Ananthakrishnan N, Chezian C, Sahai A. Truncal vagotomy and gastrojejunostomy for chronic duodenal ulcer in India. Natl Med J India. 1996;9:57-60.
2. Ahmad A. Abolition of the postprandial alkaline tide after vagotomy and its use as a screening test in assessment of vagotomy. Br J Surg. 1986;73:917-9.
3. Ramasamy R, Manohar K. Safe bedside test to assess the completeness of vagotomy. Indian J Surg. 1991;53:19-22.
4. Johnson CD, Mole DR, Pestridge A. Postprandial alkaline tide does it exist? Digestion. 1995;56:100-6.
5. Vaziri ND, Byrne C, Ryan G, Wilson A. Preservation of urinary postprandial alkaline tide despite inhibition of gastric acid secretion. Am J Gastroenterol. 1980;74:328-31.
6. Dubey D. Urinary acid output as a test for completeness of vagotomy. A dissertation submitted to the Pondicherry University, 1993.
7. Sharma MP, Ahuja V. Current management of acid peptic disorders. JIACM. 2003;4:228-233.
8. Read RC, Doherty JE. Cardiovascular effects of insulin induced hypoglycemia in man during Hollander’s test. Am J Surg. 1970;110:155-62.
9. Stempien SJ. A note on the hazards of maximal insulin testing. Gastroenterology. 1971;60:345-6.
10. Ganong WF. Review of Medical Physiology, 20th edn. Mc Graw-Hill Education. 2002:477.
11. Baron JH. Acid secretion in duodenal ulcer before and after surgery. Mt Sinai J Med. 1974;41:732.
12. Dandapat MC, Panda BK, Patra SK. Assessment of vagotomy by postprandial alkaline tide. Indian J Surg. 1991;53:8-11.
13. Rosemary J, Adithan C, Padmaja N, Shashindran CH, Gerard N, Krishnamoorthy R. The effect of the CYP2C19 genotype on the hydroxylation index of omeprazole in South Indians. Eur J Clin Pharmacol. 2005;61:19-23.
14. Thomas JE, Eastham EJ, Weaver LT. New non-invasive test of gastric secretion for use in children. Gut. 1993;34:738-41.